Sounds reasonable, until you look at the Silicon Valley experience. Silicon Valley grew like a weed precisely because employees could…
Monday Morning Update 7/13/15
Top News

St. Elizabeth’s Medical Center (MA) will pay $218,400 to settle federal charges that it violated HIPAA when employees stored patient information in an unnamed Internet file-sharing application.
Reader Comments
From Dirk Diggler: “Re: startups. I wondered what your number one piece of advice for them would be.” I could make a long list of the potholes that have consumed a bunch of companies, but I think my top item would be to understand that you can start a business without hanging the limiting “startup” label on yourself. Startups refer to companies that accept a bunch of investor money (or would like to) and therefore are wed to the concept of growing fast and big by solving a big problem before their corporate clock runs out, which requires many simultaneous talents. The risks are extensive and the chances for success are small, sort of like swinging wildly for the fences with every at bat hoping for a miracle. You can create a perfectly nice and solid business with less risk and potentially better return by just finding your niche and working it well, avoiding the temptation of giving away equity (and thus control) to investors who see things differently and who just might fire you down the road. Small business skills are very different than startup-to-IPO skills and people aren’t always good at judging which (if either) they possess. Companies should stop using the “startup” label once the initial inflated optimism has been tempered by the passage of time or the lack of traction that suggests it’s just a business, not really a startup. It’s also true that while a few companies have made it big because they had a fresh idea, it’s mostly solid execution and perseverance that trumps brilliance.
HIStalk Announcements and Requests
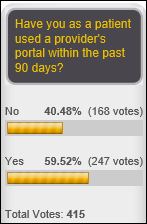
Sixty percent of poll respondents say they’ve user a provider’s portal in the past 90 days. HIS Junkie added comment, “And it was in error and was virtually useless.” New poll to your right or here: have you completed an Advance Directive?
Grammar and usage gripe: people who pronounce “chipotle” as “chipolte” even when seeing it in writing.
A note to sites that shove annoying survey pop-ups in the faces of people who might otherwise have been interested in what the site offers: my feedback is that I leave the site immediately. It’s like entering a business and being intercepted by a survey-taker even before you can get in the door to see what they’re selling. Girl Scouts know you sell cookies to people leaving the store, not those going in.
A reader asked me to describe the steps I took in trying (unsuccessfully, as it turned out) to get an electronic copy of my medical record from a hospital that should be able to provide it (EMRAM Stage 7, Epic, MU Stage 2). Here you go.
Day 1
The records request page on the hospital’s website offers two options: dropping by personally to the hospital’s HIM department (which was clearly their preference) or downloading, completing, and faxing a form (which could have been easily converted to an online form to eliminate the ridiculous faxing step). The form was complicated since it was primarily designed for patients who want to give someone else access to their records, such as for a workers compensation claim – they really should create separate forms to avoid awkward references to “the patient” when it’s the patient making the request. It also asked for the medical record number, which hospitals frustratingly expect patients to learn and remember. The form also didn’t give an option for paper vs. electronic records. It mentioned that unstated fees would be charged (hospitals are always terrible at price transparency) and that the hospital uses an outside release of information vendor that would be following up. It didn’t ask how I would like to be contacted.
Day 11
I called HIM since I had heard nothing about my request. They said they hadn’t done anything because I hadn’t provided dates of service for my one and only encounter with the health system (since I couldn’t remember the date). They looked it up and said they would mail the records. I told them I wanted them in electronic form. The HIM person said they don’t provide electronic information to patients, only to physicians. I said they were obligated to do so and she said she would get back with me after talking to her supervisor.
I called the hospital’s Epic MyChart support to see if I could download my records. They created an account for me, but it did not show any hospital admissions even though the labs from my very short stay were listed. A couple of issues might have caused the average patient to stumble – the support page wasn’t consistent in terminology (“activation code” vs. “access code”) and MyChart was fragmented between inpatient and outpatient visits with links to jump from one to the other (“visit” versus “inpatient admission.” The login page also didn’t render correctly in Firefox.
I entered a MyChart system message asking the hospital to check on why my admission wasn’t visible. It promised a response within two business days. I still haven’t received one.
Day 13
I called the hospital’s MyChart support number again. The tech was clearly not even seeing the same screens I was since she tried to walk me through finding my admission. None of the tabs or menu options she asked me to click were present. She mentioned a link she was seeing called “MyChart Administration” and I asked if perhaps she wasn’t logged in correctly since that didn’t seem like an option a patient would see. She was confused and could not understand why her screens didn’t match mine. We gave up at that point and she offered no alternative.
I hadn’t heard back from HIM, so I called them again. The supervisor repeated that they are not obligated to give patients electronic copies of their records and would provide only mailed paper copies. I repeated that they are obligated to do so and she got kind of snotty in telling me I was wrong. I filed a complaint with the Office for Civil Rights.
Day 17
I haven’t heard anything from the health system or OCR. I’m glad I didn’t need the records urgently.
My conclusions so far:
- Hospitals are not good at consumer-facing interactions. HIM people speak their own language and the records request process was developed for their convenience, not that of the patient. It’s inconceivable that hospitals expect patients to drive to their location, find a parking spot and pay for it, navigate their way through the inevitable wayfinding maze to find the HIM department, fill out a form in person, and then leave having accomplished nothing more than dropping off a paper form since the records have to be mailed later anyway.
- Hospitals seem really puzzled that the average patient doesn’t have a fax machine since they have them everywhere (hospitals are the last holdout for antique technologies such as numeric pagers and tube TVs).
- MyChart is really cool. I had another health system’s version of it and this one had a lot more functionality and was very slick. That wasn’t much help since my admission wasn’t listed and the hospital support people didn’t respond to my MyChart message.
- It was odd to me that as I was demanding electronic copies of my records, the HIM person didn’t mention MyChart at all. The hospital’s HIM and IT people should get together and make sure patients know their options either way – why wouldn’t the poorly designed HIM web page and request form tell patients that MyChart access might be all they need instead of paying for paper copies and waiting for them to be delivered?
- The HIM people don’t know much about the health system’s obligations to provide electronic copies, having rather smugly told me I was incorrect in believing they are required to do so.
- Perhaps other providers could get copies of my records quickly in an emergency, but I wouldn’t count on it. I’m not even sure they would bother trying because they know what a pain it is – they would simply carry out their treatment without any knowledge about me that exists elsewhere. During that very short admission, which included a couple of hours in the ED, I mentioned that my records were in my out-of-state hospital’s Epic system and as far as I know they didn’t try to get them.
Last Week’s Most Interesting News
- CMS announces that its latest round of testing produced zero ICD-10 errors from test claims submitted by volunteers, concluding that it will be ready for the October 1 switchover.
- An investigation of CMS’s National Provider Identifier finds many errors, some of them suggesting that providers with a checkered medical past intentionally used the NPIs of other providers to avoid being exposed on consumer doctor rating sites.
- CMS agrees to the AMA’s demand for a year-long ICD-10 transition period for physician practices in which it will accept less-specific ICD-10 codes and provide advance payments its systems malfunction.
- Aetna announces that it will acquire Humana for $34.1 billion pending FTC approval, a deal that carries technology implications since both companies have health IT offerings.
Webinars
July 14 (Tuesday) noon ET. “What Health Care Can Learn from Silicon Valley.” Sponsored by Athenahealth. Presenter: Ed Park, EVP/COO, Athenahealth. Ed will discuss how an open business structure and strong customer focus have helped fuel success among the most prominent tech companies and what health care can learn from their strategies.
July 22 (Wednesday) 1:00 ET. “Achieve Your Quality Objectives Before 2018.” Sponsored by CitiusTech. Presenters: Jeffrey Springer, VP of product management, CitiusTech; Dennis Swarup, VP of corporate development, CitiusTech. The presenters will address best practices for building and managing CQMs and reports, especially as their complexity increases over time. They will also cover quality improvement initiatives that can help healthcare systems simplify their journey to value-based care. The webinar will conclude with an overview of how CitiusTech’s hosted BI-Clinical analytics platform, which supports over 600 regulatory and disease-specific CQMs, supports clients in their CQM strategies.
Previous webinars are on the YouTube channel. Contact Lorre for webinar services including discounts for signing up by July 31.
People

Patrick Swindle, manager of IT systems support at East Texas Medical Center, is promoted to administrator of ETMC Quitman.
Innovation and Research
The Seattle business paper profiles University of Washington spinoff C-SATS (which stands for crowd-sourced assessment of technical skills), which evaluates surgeons by having videos of their procedures reviewed by experts. Some of the executive team members came from Classmates.com. The company just raised $2.5 million.
Technology
A site claiming to have inside information about the next version of Google Glass – marketed to enterprises, not consumers – says it will include a larger prism, more processing power, better battery life, and support for 5 GHz band video streaming. The move to enterprise is smart since Glass was never going to be socially acceptable in public, but that shouldn’t be a problem where the role of its user is known, such as a patient seeing a doctor wearing Glass. It will still be geeky, but at least less creepy.
Other
Cerner responded to my question about the DoD’s CoPathPlus award that was announced last week. It was a new procurement outside of the DHMSM award, which was obvious, but more importantly it was not a renewal of DoD’s previous CoPath contract or an upgrade to that product. It still seems odd that both Cerner and Sunquest sell CoPathPlus and that Sunquest sells two anatomic pathology products.
A Caribbean newspaper profiles Modernizing Medicine software consultant Chantel Kelly, who was so moved by pleas for supplies in Jamaica’s hospitals that she personally bought bed linen for all of Kingston Public Hospital. Surgeons say they’re operating wearing plastic bags instead of surgical aprons because it’s all they have, so Kelly says she will buy them surgical and patient gowns next.
A front-page New York Times article reviews virtual visits and the increasing number of insurers willing to pay for them, noting that they cost a lot less than in-person visits but adding that they may drive up overall healthcare costs since the patients might just have stayed home untreated with self-limiting conditions otherwise (an excellent point). A first-time virtual visit patient with a toothache reports her experience as, “I was in so much pain, I didn’t care that it was weird. He got right to the point, which was what I wanted. He prescribed antibiotics and called them into an all-night pharmacy about 20 minutes away.” The article uses the term “virtualist” to describe physicians who provide video visits.
In England, NHS warns ambulance trusts to keep their GPS map software updated after two patients died when drivers couldn’t find their home addresses, with at least nine reports of patient safety issues related to outdated map files.
Non-profit investigative journalism organization ProPublica announces that it will release a “Surgeon Scorecard” next week based in its analysis of Medicare complication rates.
The Detroit oncologist who admitted giving chemotherapy to more than 500 cancer-free patients to defraud Medicare and insurance companies of dozens of millions of dollars is sentenced to 45 years in prison.
Lee Memorial Health System (FL), whose certificate of need request to build a new hospital was turned down by the state after a competitor’s complaint, will instead spend up to $140 million to build a hospital without beds. The campus will include a freestanding ED, outpatient surgery center, an imaging center, lab, and medical office space, all tied together by its Epic system and centralized scheduling.
Sponsor Updates
- Sunquest Information Systems will hold its Executive Summit and UGM July 13-17 in Scottsdale, AZ.
- TeleTracking offers “Patient Discharges – a Stumbling Block to Patient Access.”
- Zynx Health posts “Improving Quality and Reducing Disparities in Care Coordination.”
- Surescripts offers “FHIR: A SMART Solution for Interoperability?”
- Surgical Information Systems offers “Why Should you GO to GO!2015? The NEW SIS User Meeting.”
- T-System posts “Leading with Passion: Hope is Not a Strategy.”
- Verisk Health publishes “Calculating Risk Scores for Dual Eligibles Under the Medicare Risk Adjustment Model.”
- Versus Tech client EMMC Cancer Care wins an ACCC Innovator Award for its use of RTLS technology.
- VisionWare will exhibit at the Healthcare Analytics Symposium July 13-15 in Chicago.
- Xerox Healthcare will host a Google+ Hangout on population health management July 16.
- ZirMed offers “An ICD-10 Code List Just for You, America.”

Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.






re: Dirk Diggler / Startups… My advice – it is mandatory that you go to market with a key hospital client as a partner, even if you have to give them equity or free software/services in exchange for references. Demonstrate success there and stay focused like a laser making them happy. With that key lighthouse customer, you might open doors. You’ll likely starve of cash waiting for the industry to move so be prepared for a roller coaster of disappointments. Avoid partners like the plague (they do not have your best interests at heart) and beware of EMR vendors and CIOs stealing your ideas to build similar solutions in-house. This industry and business in general is full of unethical people.
RE: pronouncing things incorrectly on-purpose as in chipolte. I refuse to correct the little dislectic brownie in my head and pronounce kanye west as ‘can-yay’. I much prefer ‘caine’. Does that make me a bad person?
[From Mr H] I usually call Citizen Kanye names that are less pronounceable (at least in polite company), but to really annoy him, I would just call him Puff Daddy.
Re: Electronic copies of your medical records.
Epic requires all clinical customers to be licensed for Lucy and MyChartCentral which allows patients to just download at least a summary of the information on their chart for any organization they have a MyChart account with. This would be accessible under Other Resources > Lucy/MyChartCentral from within MyChart. This doesn’t cost the org anything extra up front (since it’s a part of a package deal orgs already have to buy if they want to buy anything), costs the orgs very little ongoing (since Epic runs the servers for it), and doesn’t take any great effort to turn on (since it’s supposed to be turned on at install and even if it isn’t there’s a utility that will do the config automatically). That said, it can be turned off, but if it is turned off I think that says quite a bit about the org’s attitude towards patients getting copies of their chart.
RE: pronouncing things incorrectly (not on purpose). I’m amazed that people who can pronounce the word ‘risk’ cannot pronounce the last syllable of ‘asterisk’ correctly. How is that possible?
So St Elizabeth’s hospital in MA is fined by the federal government for a HIPAA violation – putting records on a file sharing service. How much is the government being fined for letting millions of confidential employee records gettin the hands of Chinesse hackers? How much Hiliary Clinton being fined by using her personal email server to conduct US State department business?