Sounds reasonable, until you look at the Silicon Valley experience. Silicon Valley grew like a weed precisely because employees could…
Monday Morning Update 6/8/15
Top News

CSC will pay $190 million to settle SEC charges of accounting fraud related to its money-losing NPfIT contracts with the UK’s National Health Service. Five of eight former CSC executives have settled SEC charges of manipulating financial results, with former CEO Michael Laphen agreeing to return more than $4 million in compensation under the clawback provision of the Sarbanes-Oxley Act. The SEC’s investigation found that CSC lied about earnings after falling short of revenue due to missed NPfIT deadlines and also took out high-interest loans from NHS to hide cash flow problems from investors. A Bloomberg report says HP was close to acquiring CSC last month for $9.3 billion but backed out, with CSC’s new plan being to split itself into two publicly traded companies.
Reader Comments
From ICDelightful: “Re: ICD-10. Why didn’t CMS just do ICD-9 to ICD-10 mapping itself to provide a single standard? Even if 20 percent of the codes don’t directly it seems like CMS is in the best position to determine which are the closest match.” I’ll leave it to more HIM-savvy readers to respond, with my guess being that ICD-10 codes have a mandatory additional level of specificity that can’t be automatically and accurately derived from a given ICD-9 code.
From The PACS Designer: “Re: coining a new term. With the advent of cloud-based solutions, it’s becoming apparent that data stored in the cloud and other database solutions need a better term than big data. With transparency being key to move data more efficiently, it would be better to use the term ‘dataware’ to describe the transparent data sources.”

From Mountain High: “Re: Boulder Community Hospital. Goes down again, this time for only about a day (eight days of downtime in 2013).” It sounds to me like they were experiencing some kind of denial-of-service or malware attack given that the forwarded internal email suggests that its network was overloaded and the IT security director was assigned to investigate.
HIStalk Announcements and Requests
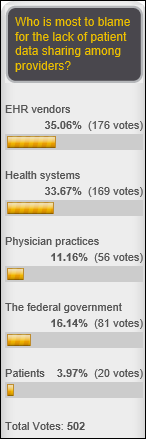
Poll respondents are equally split as to whether lack of patient data-sharing should be blamed on health systems or their EHR vendors. Will says the correct answer is none of the above – the fee-for-service system treats interoperability as an unreimbursed cost and data will be shared when there’s a business reason to do so, while Frank blames lack of customer (patient) demand and Mobile Man says the biggest payor (Uncle Sam) could change interoperability overnight by changing reimbursement. New poll to your right or here: how will overall health IT vendor revenue change over the next five years?
My latest grammar peeve: capitalizing relationship names when the word isn’t used as a title, as in, “I visited my Dad” (wrong) vs. “I visited Dad” (right). Sometimes people mysteriously do the same in referring to an occupation, such as “I am a Teacher.” Not new but increasing in frequency is the practice of combining words not used as adjectives, such as, “I brush my teeth everyday” (wrong) vs. “My everyday practice is brushing my teeth” (right). I acknowledge that rampantly incorrect word usage will eventually find its way into dictionaries that see their role as observational rather than authoritative, which would make one fine mess in nearly every other discipline where things are either right or they aren’t despite what the questionably knowledgeable masses believe.

Mrs. H says the two Chromebooks we bought for her Oregon elementary students via the DonorsChoose project (with matching funds from the Bill & Melinda Gates Foundation) have boosted morale and improved reading scores. I have $10,000 in matching money available (courtesy of an anonymous vendor executive’s personal pledge) for companies donating $1,000 or more, who also get a mention right here on HIStalk for their involvement.
Last Week’s Most Interesting News
- Quality Systems President and CEO Steven Plochoki resigns.
- BIDMC CIO John Halamka, MD urges CMS to shut down the Meaningful Use program and instead hold providers accountable for patient outcomes and letting the market determine which technologies they need.
- A M&A publication states that health IT firms Netsmart, Precyse Solutions, Mediware, Edifecs, Caradigm, and Altegra Health are being shopped for sale.
- A cybersecurity firm warns that unsecured medical devices provide hackers with a nearly undetectable back door into health system networks.
- Partners HealthCare (MA) goes live on Epic at a total project cost of $1.2 billion, double its original budget.
- An insurance company demands that Cottage Healthcare System (CA) repay its $4.1 million breach settlement, saying the hospital lied on its insurance application by claiming it was performing IT security maintenance steps when it really wasn’t.
- A Texas judge issues an injunction requested by telemedicine vendor Teladoc against the Texas Medical Board for its requirement that physicians conduct an initial face-to-face patient visit before prescribing drugs.
Webinars
June 9 (Tuesday) 11:30 ET. “Successful HIEs DO Exist: Best Practices for Care Coordination.” Sponsored by Medicity. Presenters: Dan Paoletti, CEO, Ohio Health Information Partnership; Brian Ahier, director of standards and government affairs, Medicity. Not all HIEs are dead – some, like Ohio’s CliniSync HIE, are evolving and forging a new path to successful care coordination. Brian Ahier will explain how HIEs can help providers move to value-based care models, emphasizing Meaningful Use Stage 3 and FHIR. Dan Paoletti will provide best practices in describing CliniSync’s journey to success in serving 6,000 primary care physicians, 141 hospitals, and and 290 long-term and post-acute care facilities. Attendees will learn how to use a phased approach, establish client champions, help providers meet MU Stage 2, create a provider email directory, deliver care coordination tools, and drive continued ROI.
Acquisitions, Funding, Business, and Stock
Shares of Evolent Health closed Friday up 11 percent to $18.86, valuing the newly NYSE-listed company at $950 million. UPMC’s stake is worth $278 million, while CEO Frank Williams holds $22 million in shares.
Glytec announces that 13 health systems have chosen its eGlycemic Management System for managing glucose levels using evidence-based insulin dosing recommendations. Among the new clients are Kaweah Delta Health Care District (CA), Edward-Elmhurst Healthcare (IL), Mary Hitchcock Memorial Hospital (NH), and Mission Health System (NC).
Government and Politics
Hawaii will shut down its $130 million health insurance exchange and move to Healthcare.gov. Hawaii’s high percentage of insured citizens, driven by a mandatory state employer insurance law, gave it too few users and too little revenue to sustain itself once it spent all of its federal grant money.
Privacy and Security
China-based hackers breach the US federal government’s personnel system and steal the information of up to 4 million current and former federal employees in a just-announced December 2014 incident. Investigators say the cybercriminals, who may be working for the Chinese government, are likely the same ones who recently breached health insurers Anthem and Premera Blue Cross. The message is clear – in-depth information about people is more desirable to hackers (or “actors,” as the security people inexplicably say) than credit card files, and the fact that the Anthem and Premera data hasn’t hit the black market would suggest that a bigger and more organized plan is in place that goes beyond simply making a quick buck. Credit cards can be cancelled after a breach, but in-depth personal information can’t.
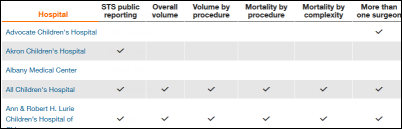
St. Louis Children’s Hospital (MO) says CNN misled readers by including it in an article titled “Is your pediatric heart hospital keeping secrets? We have answers.” The hospital says the CardioAccess software it uses doesn’t collect all of the information, leaving the hospital unable to report it.
Reno, MV pediatrician Ron Aryel, MD says syndicated columnist and non-practicing physician Charles Krauthammer is wrong in blaming physician dissatisfaction on EHRs. “My electronic medical record is my most powerful tool in the office. It helps to organize my thinking, prevents mistakes, and helps me spot important trends within my practice. My time ‘entering data’ rewards both me and my patients with better outcomes and more effective medicine. But doctors should focus on what they do best. I am good at getting patients healthy, and Krauthammer is good at being paid to write opinion pieces. I think he should keep doing that.” Krauthammer might not even be all that good at writing opinion pieces – he doesn’t offer one shred of proof to back up his assertion that an “EHR mandate” is causing physicians to quit. Nobody “mandates” that physicians accept insurance, deal with Medicare, sell their practices to health systems, or use EHRs – they voluntarily did all of those things for the money and now have seller’s remorse, leaving them with three basic choices: (a) deal with it while complaining to anyone who will listen; (b) start over in a cash-only concierge practice; or (c) quit and do something else. The problem with (c) is that doctors nearly always find the market value of their non-medical capabilities to be much less than they themselves believe, with the threatened loss of income and status steering them back to (a) in most cases. Actually I don’t have any more data than Krauthammer cites, but I suspect there’s a (d) choice in which doctors take purely transactional 9 to 5 physician jobs, such as working for insurance companies, telemedicine providers, consulting companies, and contracted physician staffing firms, accepting the notion that doctors rarely hang out their own shingles these days and that means becoming a begrudgingly obedient time-selling corporate widget like most everybody else who doesn’t drape a stethoscope around their neck as a status symbol.
Here’s yet another questionably useful gadget for quantified selfers to embrace: The Lovely, a wearable sex tracker / sex toy (already tagged as the “Fitbit for your penis”) whose app tracks intensity and calories burned and provides suggestions for improvement and experimentation. I’m fearful of a future in which lust-crazed users flood Facebook with their Lovely-generated updates and boastful historical dashboards.
Weird News Andy says this spine transplant wasn’t about politicians, but rather a 35-year-old woman who faked romance with an 86-year-old man and then scammed him into giving her $1.2 million to pay for her “spinal transplant.” WNA’s rim shot conclusion is that “her story really struck a chord with the victim.”
Sponsor Updates
- Zynx Health offers “Restricting Low-Volume Hobbyists: Translating the Volume-Outcome Relationship Into Health Policy.”
- Streamline Health will exhibit at the 2015 CHIA Convention & Exhibit June 8-10 in Palm Springs, CA.
- Sunquest releases the agenda for its 2015 Executive Summit July 13 in Scottsdale, AZ.
- Xerox Healthcare offers “Healthcare C-Suite Sets Sights on Population Health Management.”
- SIS COO Doug Rempfer pens an article for HFMA’s magazine entitled, “Using Perioperative Analytics to Reduce Costs and Optimize Performance in the OR.”
- T-System offers “Leading with Passion: Checking in on Your People.”
- TeleTracking will exhibit at the Digital Health and Care Congress 2015 June 16-17 in London.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.







If we’re being language sticklers, Mr. H, WNA’s punch line should be “struck a cord” not “chord”.
RE: From Mountain High: “Re: Boulder Community Hospital. Goes down again, this time for only about a day (eight days of downtime in 2013).” It sounds to me like they were experiencing some kind of denial-of-service or malware attack given that the forwarded internal email suggests that its network was overloaded and the IT security director was assigned to investigate.
It’s not necessarily a malicious DOS. It sounds to me more like a spanning tree/loop event:
http://www.cisco.com/c/en/us/tech/lan-switching/spanning-tree-protocol/index.html
Probably they made some update to one of their switches and it kept flooding as a result. It’s always scary when the networking team makes a change because even something small and/or innocuous sounding can take down an entire subnet. No Chinese hackers necessary.
Valuable comments – I learned a lot from the facts – Does someone know where my company could get access to a blank a form document to complete ?