I want to add the following. I'm an IT professional. In the course of my professional duties, I'm expected to…
Readers Write: Why Some Physicians are Opting Out of Meaningful Use Attestation
Why Some Physicians are Opting Out of Meaningful Use Attestation
By Charles Settles

Since its inception, the Meaningful Use Incentive Program (MUIP) has paid out nearly $30 billion worth of incentives, but a rising number of physicians are opting out. Why?
2011, the first year of the MUIP, saw widespread interest. Nearly 200,000 eligible providers (EPs) and over 3,000 hospitals completed registration for either the Medicare or Medicaid versions of the program, according to the latest summary report from CMS. However, much of this original momentum appears to be lost. 2014 saw under 73,000 EPs and just 108 hospitals register across both programs.
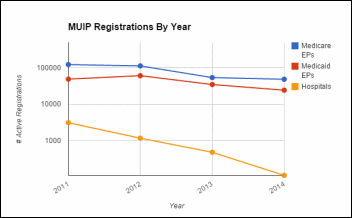
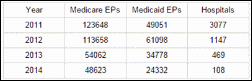
Altogether, 515,158 registrations have been completed by EPs across both programs, with 415,550 unique EPs receiving an average of $25,190 in incentive payments. According to the CMS’s latest data, just over half of eligible providers have received an incentive payment. But what about the other (at least) 40 percent?
It can’t simply be a question of eligibility. According to Medscape’s 2014 EHR Report, only 22 percent of physicians are abandoning or have never supported the MUIP, but examining the CMS summary report suggests a much higher rate of attrition — only 23 percent of the 260,900 physician EPs who received a payment in 2013 received one in 2014. That translates to an attrition rate of just under 77 percent.
When considering the payments only by stage of the program, the numbers for physicians are even worse — only 5.7 percent of those physicians who received a payment for the first stage have received one for the second. More physicians will complete Stage 2 eventually, but the odds of making it to CMS’s 75 percent adoption rate target by 2018 appear to be growing shorter. The carrot simply hasn’t been enough.
The stick may not be enough either. If the 75 percent adoption rate target is not met, reimbursements stand to be cut by up to five percent. The average family physician, arguably the primary focus of the MUIP, receives about $100,000 per year from Medicare reimbursements, according to Dr. Jason Mitchell, former director of the American Academy of Family Physicians’ Center for Health IT. Since the penalties increase by one percent per year beginning with a one percent penalty in 2015, a physician receiving $100,000 annually could lose up to $10,000 in reimbursements through 2018. For some, the penalty is a small price to pay to not have to deal with requirements that they feel prevent them from delivering better patient care.
Dr. S. Steve Samudrala, medical director of America’s Family Doctors, was an early proponent of electronic health records, patient engagement, and other medical software systems. It seems ironic that Dr. Samudrala does not participate in the MUIP. Though his EHR (eClinicalWorks) is fully certified through Stage 2, Dr. Samudrala feels the reporting requirements for primary care physicians would prevent him from delivering the high quality, personal care his patients have come to expect.
He does acknowledge, though, that many independent primary care physicians have little choice in the matter — the incentives can make or break some smaller practices. Payments are shrinking, competition from hospital-owned groups is increasing, and medical practice brokers keep calling. Dr. Samudrala’s bet isn’t on incentives — he and a growing number of primary care physicians are proponents of what’s coming to be known as “direct primary care.”
The idea behind direct primary care, sometimes called “concierge medicine,” is to remove the expensive bureaucracy and processes associated with billing insurance or government programs and offer services directly to patients for a monthly or annual fee, supplemented by small co-pays. Though the number of successful direct primary care practices is small, and the trend doesn’t solely explain the number of physicians opting out of the MUIP, rising interest in the concept makes it worth mentioning.
Ultimately, the MUIP will likely be viewed as a success if widespread adoption of health IT was the goal. Adoption doubled between 2009 and 2013. Even if physicians don’t meet all the requirements to receive incentives, the benefits of health IT to providers, payers, and most importantly patients cannot be denied. We’ll likely see even more attrition from the MUIP with the announcement of the Stage 3 rules, but despite the growing disillusionment with the program, EHR and other health IT is here to stay.
Charles Settles is a product analyst at TechnologyAdvice.


No need to look at carrots, sticks, or eligibility. Just ask some docs and nearly all will say the same thing: MU now simply requires too much time-consuming, pointless documentation, and provides little or no improvement in patient care or efficiency. Many of us were willing to give it a shot at first, but the benefit just isn’t there for most of us or for our patients.
Good point, same (even more so) is true for hospitals.
If you run the numbers for a typical community hospital it might get up to a $200k penalty/yr. That’s peanuts on a $150+ milion budget, not to mention the costs of the EHR ($10+ million) and costs of MU compliance and audits.
As I’ve posted on this blog and others – do it for real business reasons, and do it on your schedule not some gung-ho regulator’s.
Excellent review. As a front line EP that has opted out of MU, I do use a non certified EHR, that is customized to my workflow and patients. Certified EHRs are one size fits none. And the MU program is a disaster for most front line EPs. There is no meaningful use of them. They are prescriptive and click here not there inefficient unsafe unusable mess. Good luck asking for workflow help. You mean a endocrinologist is not the same as a ob gyn or orthopaedic surgeon? Not sure what the overall goal is for ONC and CMS, but it seems that they want all private practice EPs out of the program. The big costs of EHR are now coming as the incentives are burned up and penalties are in effect, which will essentially kill MU this year or next. I find it strange to listen to HITPC meetings where they all backslap each other about the MU program and its success. I would challenge you to find a single front line EP that thinks that. MU 3 is a unmitigated disaster and essentially speaks volumes on the tone deaf nature of ONC and CMS. If MU is so great, where are all the savings? the better care? The happy patients? My suggestion, let EPs in the interop program with any EHR. No certification. Let the vendors actually build software for us instead of MU. Forget all other check boxes and objectives and measures. Just let the market do the work for interop. If patients and EPs want it, we will demand it and pay for it. To force it with an artificial market, never works. Lets all just hold hands, look at each other and say, “its ok, MU is dead.” We have to stop the silliness and actually listen to EPs.