I want to add the following. I'm an IT professional. In the course of my professional duties, I'm expected to…
News 4/11/14
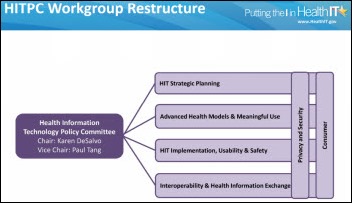
ONC head Karen DeSalvo proposes dissolving the agency’s workgroups and forming four new ones in order to reduce redundancy and create a “less siloed” approach. The proposed workgroups would focus on (a) health IT strategic planning; (b) advanced health models and Meaningful Use; (c) health IT implementation, usability, and safety; and (d) interoperability and health information exchange.
Reader Comments
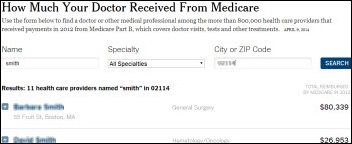
![]() From Jeff: “Re: Medicare reimbursement data. If you use the New York Times tool, it becomes very, very easy to look up your local docs and their payouts.” CMS released Medicare payment data on Wednesday on 880,000 providers who collectively received $77 billion in Medicare payments in 2012. I struggled to manipulate the data using Excel, but it took me just seconds to look up details on all my doctors (and a few doctor friends) using the Times tool. While I understand why doctors aren’t happy that the world can now see much of our tax dollars ended up in their individual bank accounts, the potential analytics value of the data is pretty exciting.
From Jeff: “Re: Medicare reimbursement data. If you use the New York Times tool, it becomes very, very easy to look up your local docs and their payouts.” CMS released Medicare payment data on Wednesday on 880,000 providers who collectively received $77 billion in Medicare payments in 2012. I struggled to manipulate the data using Excel, but it took me just seconds to look up details on all my doctors (and a few doctor friends) using the Times tool. While I understand why doctors aren’t happy that the world can now see much of our tax dollars ended up in their individual bank accounts, the potential analytics value of the data is pretty exciting.
From Lincoln: “Re: Medicare reimbursement data. What’s your take, Mr. H?” The government didn’t release the data until forced, so chalk up one for the Freedom of Information Act and the responsible publications that pressed the issue. I agree with Inga that the information is interesting, but I think it will raise more questions than it answers. The public doesn’t realize how screwed up Medicare payments are, so the nuances of payments made to groups, doctors being paid directly for administering drugs, and other quirks are going to sail right over their heads. CMS isn’t known for outstanding customer service, so who’s going to answer that deluge of questions about specific examples that are so easy to find? Probably the high-earning providers themselves, who are getting calls from their local papers looking for a hot story. What will they say about Medicare rules allow a single specialist to crank out enough high-paying procedures to earn many millions vs. primary care guys barely making a living – it’s better than fraud, but brings up the whole value question that CMS encourages by paying heavily for procedure medicine. I’m also annoyed at the CMS insinuation that citizens should help them fight fraud – why don’t some of their bureaucrats who understand the rules and are paid to enforce them look at the information themselves and realize that paying some doctor $20 million in a single year might be cause for concern instead of waiting for amateur SAS jockeys to point that out? Our “pay and chase” system is great for providers and great for hiding government inefficiency that would manifest itself as infinitely delayed payments, but it’s not so great for taxpayers. Patients don’t even know what is being billed and paid on their behalf and checks and balances are non-existent. The great thing about releasing this information is that everybody should be embarrassed at the sorry state and high cost of government-funded healthcare, especially the politicians who let it happen.
From CIO D: “Re: eating your own dog food. Here’s our policy on PC lockdowns. If the PC is used predominately by one person (i.e. that’s Joe’s Computer) it is NOT locked down. If the PC is used publicly by many people (i.e. at a nurse station or in a patient room) it is locked down. I think that’s a fair way to handle it.”
HIStalk Announcements and Requests
![]() A few highlights from HIStalk Practice this week include: satisfaction is climbing among primary care EHR primary care users that implemented their system more than two years ago, according Black Book Rankings. Why I found a Huffington Post article on patient etiquette offensive. CVS wants MinuteClinic to complement and support the broader healthcare landscape. The PQRS and e-Rx program saw sharp increases in physician participation in 2012. CMS offers a Stage 2 MU Attestation Calculator to assess readiness. Independence Blue Cross and DaVita launch a new healthcare business model aimed at reducing care costs. Securing a new-patient appointment is easier for individuals with private insurance. Culbert Healthcare Solutions’ Brad Boyd discusses three factors for success in using informatics. Thanks for reading.
A few highlights from HIStalk Practice this week include: satisfaction is climbing among primary care EHR primary care users that implemented their system more than two years ago, according Black Book Rankings. Why I found a Huffington Post article on patient etiquette offensive. CVS wants MinuteClinic to complement and support the broader healthcare landscape. The PQRS and e-Rx program saw sharp increases in physician participation in 2012. CMS offers a Stage 2 MU Attestation Calculator to assess readiness. Independence Blue Cross and DaVita launch a new healthcare business model aimed at reducing care costs. Securing a new-patient appointment is easier for individuals with private insurance. Culbert Healthcare Solutions’ Brad Boyd discusses three factors for success in using informatics. Thanks for reading.
This week on HIStalk Connect: Dr. Travis discusses CRM for healthcare and the shift within emerging healthcare startups to focus on technology that enhances the doctor-patient relationship rather than building patient engagement apps. HIStalk Connect’s Q1 Digital Research Recap highlights some positive findings across telehealth, patient portals, and EHR-driven outcomes research. Scanadu halts shipments on its Indiegogo-backed, tricorder-like Scanadu Scout.
Upcoming Webinars
April 16 (Wednesday) 11:00 a.m. ET. Panel Discussion: Documents, EMRs, and Healthcare Processes. Sponsored by Levi, Ray & Shoup. Presenters: Charles Harris, senior technical lead, Duke University Health System; Ron Peel, technical advisor, LRS; and John Howerter, SVP of enterprise output management, LRS. IT department in hospitals implementing EMRs often overlook the role of document-driven workflows. Prescriptions, specimen labels, and discharge orders, and other critical documents must be reliably delivered with minimal impact on IT and clinical staff. This panel discussion will discuss the evolving use of documents in the “paperless/less-paper” environment.
Acquisitions, Funding, Business, and Stock
Minneapolis-based Healthcare Engagement Solutions, which offers physician collaboration tools, closes a $550,000 angel investment.
Drchrono secures $2.69 million in convertible debt funding, bringing the company’s total to $6.77 million.
Sales

Enclara Health will implement CoverMyMeds to automate prior authorizations in its hospice pharmacies.

Lakeland Regional Health Systems (FL) will expand its use of Allscripts ambulatory EHR and PM, use the company’s managed services, and implement its Payerpath financial management software.

Capital Regional Medical Center (MO) selects Patientco as its patient payment automation solution.
Health information organization SacValley MedShare (CA) selects ICA as its HIE vendor.

Deaconess Health System will integrate its network with Availity for clearinghouse and RCM services at five of its southern Indiana hospitals, 20 primary care clinics, and several specialty facilities.
![]()
The Greater Houston Healthconnect selects DICOM Grid to electronically deliver medical images to area hospitals and physicians at the point-of-care.

Bay Area Medical Center (WI) signs a three-year agreement with Zix Corporation for email encryption.
People

Kareo names Tom Patterson (Teletrac) CFO.
Nextech hires Rhonda Russell (McKesson) as COO.
Carl Byers (Fidelity Biosciences) joins the board of Cureatr.
IMedicor promotes Srini Vasan from SVP of technology to CTO.
Announcements and Implementations
Dignity Health, Box, and The Social+Capital Partnership name WelVU the winner of their developer challenge for personalized patient engagement solutions. WelVU, which allows providers to create customized educational videos during appointments, received a $100,000 convertible note and one-month office space and mentoring.
New Jersey Health Commissioner Mary E. O’Dowd announces the launch of the New Jersey HIN, which connects six regional health information organizations and 9,000 providers.

Wesley Medical Center (KS) adds Lincor’s LINC Technology platform for patient engagement and entertainment to newly updated patient rooms.
Government and Politics
ONC renews its Cooperative Agreement with DirectTrust, a non-profit trade alliance that promotes secure HIE via Direct Protocol.
Technology

The folks at Vonlay remind Epic users that while the Heartbleed OpenSSL vulnerability doesn’t affect MyChart or EpicCare Link because Microsoft’s IIS isn’f affected, the non-Epic parts of the setup might be, such as the load balancer. Web servers can be checked here, assuming the guy who developed the page knows what he’s doing.
Other
An Institute of Medicine report recommends including information about patients’ social influences and behavioral habits in their EHRs to improve outcomes and advance public health research efforts.

HHS OIG reverses a 2011 advisory opinion that had allowed athenahealth to charge $1 to providers not on the athena network for processing their test orders, saying the arrangement could violate anti-kickback statutes. The termination means that athena can no longer discriminate between in-network and out-of-network providers and will therefore charge $1 for all orders. Athenahealth calls the reversal a “setback” for sustainable HIE.
Third-party ACO vendors outperform EMR vendors when it comes to meeting the needs of physician-led ACOs, according to KLAS. Epic and eClinicalWorks earned the top scores among EMR vendors in meeting physician needs.
Researchers at the UK’s Birmingham Women’s Hospital find that doctors save an hour per day using a tablet vs. paper.
![]() I never cease to be amazed by physicians who totally ignore the business side of their practices. Case in point: a Pennsylvania woman, whose job duties included making bank deposits for her physician employers, is charged with stealing $106,000 over a six-year period, the time it took for anyone to notice that the deposits didn’t match collections.
I never cease to be amazed by physicians who totally ignore the business side of their practices. Case in point: a Pennsylvania woman, whose job duties included making bank deposits for her physician employers, is charged with stealing $106,000 over a six-year period, the time it took for anyone to notice that the deposits didn’t match collections.
Weird News Andy might have been predictable in titling this story “Nothing to sneeze at.” An MIT study finds that cough and sneeze droplets may travel up to 200 times further than previously thought, which should be comforting to think about when you hear that guy hacking up a lung 10 rows back on the plane.
Sponsor Updates
- Visage Imaging announces Version 7.1.5 of its Visage 7 Enterprise Imaging Platform.
- CCHIT certifies NextGen Emergency Department Solution version 6.0 as a ONC 2014 Edition criteria EHR module.
- HCI Group launches the HCIsustain service line to provide long-term EHR support.
- Greenway Health partners with TrustHCS to assist PrimeSUITE users with their ICD-10 preparation and transition.
- InterSystems will showcase its healthcare solutions and technology at the Ministry of Health and HIMSS Middle East Conference next week in Saudi Arabia.
- T-System CMIO Robert Hitchcock, MD is re-elected to the Emergency Department Practice Management Association board.
- Coastal Healthcare Consulting selects Divide to build its BYOD program.
- Holon is participating in this week’s Texas Organization of Rural and Community Hospitals Annual Conference & Trade Show in Dallas.
- Elsevier Clinical Decision Support posts two short, fun videos explaining how InOrder sets improve quality of care.
- MaineGeneral Health equips its newly-opened Alfond Center for Health with Versus RTLS and seven Versus applications.
- Coastal Healthcare Consulting offers a case study highlighting their data extraction project with Nebraska Medical Center.
- Marla Simmet, executive consultant for Beacon Partners, shares tips for surviving a MU audit on the company’s blog.
- Perceptive Software introduces Content 7, the latest version of Perceptive’s enterprise content management technology.
- UNC Charlotte and Premier partner to develop tools aimed at helping providers improve population health.
EPtalk by Dr. Jayne
The hot news in the physician lounge (and in the elevator, the parking garage, and the locker room) this week was the publication of the Medicare physician payment data. Most of the websites I looked at played up the sensational aspect – the 344 physicians who received more than $3 million in payments in 2012. The AMA and other organizations have tried to block access to the data, citing physician privacy concerns and the potential for inaccurate information. Patient advocacy and consumer groups argue that the data will help the public identify providers who provide quality, cost-effective care.
I looked at the data in a couple of different formats:
- The data files directly available from CMS
- The New York Times site
- The Wall Street Journal site
I searched not only for myself in the database, but several of my friends and quite a few physicians who make me crazy at work. Just from eyeballing, I can see that there may be issues with the data. My OB/GYN BFF was cited as receiving barely more than $1,000 from Medicare – 18 breast exams and 15 pap smears. I’ve seen her data in our billing system and she saw (and was paid for) many more Medicare procedures in 2012 including hysterectomies, endometrial biopsies, and more. She doesn’t participate in Medicare Advantage plans, so I’m not sure why there are amounts missing.
In my opinion, the Wall Street Journal site had the best explanation about the data and what it does or does not represent. In short:
- It may not present the full picture about a physician’s practice and its revenue
- The complexity and similarity of CPT codes make it hard to compare physicians
- Physicians may have been paid for others working under their supervision
- Physicians caring for complex patients may be paid more
- It doesn’t include Medicare Advantage payments or procedures that a physician performed on 10 or fewer patients, nor does it include payments for services billed under an employer’s provider number
- Physicians who bill for imaging or other high-overhead services may receive higher payments
- Medicare payments are different across the country
The New York Times site had an explanation about the source data, but it wasn’t nearly that comprehensive. One CMS administrator was quoted as saying, “We want the public to help identify spending that doesn’t make sense.” I’m not sure how providing the data as it currently exists would help the general public decide whether it makes sense or not.
The payments also include reimbursements for drugs – from flu shots to high-dollar chemotherapy agents. Depending on the specialty and type of drug, the physician may be receiving anywhere from less than the cost of the drug to a significant markup or even rebates.
Major institutions including the Cleveland Clinic, the Mayo Clinic, and the University of Michigan Health Systems issued statements explaining how some of their physicians are compensated. Many are employed physicians. Others may be part of project such as the Michigan Primary Care Transformation demonstration project, where the director was tagged for more than $7.5 million in payments for 207,000 patients cared for by 1,600 physicians.
Given the nature of the data released, I don’t see how anyone could extrapolate quality of care or cost effectiveness. I would be concerned, though, if my physician was an outlier among those in the same area or specialty. Looking at one of the physicians who makes me crazy at work, he received more than four times the amount of payments of some of his colleagues. I know that he sees an insane amount of patients, works 12-14 hours a day six days a week, and is essentially a robot. His patients know he’s a robot because he refuses to address more than one patient concern in a single visit. Knowing those facts, maybe his numbers make sense.
If you’re a physician, did you look at your own data? Did you look at that of your peers? If you’re in IT like me, did you check out the physicians based on whether they are naughty or nice? What’s your take on the data? Email me.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis, Lorre.
More news, HIStalk Practice, HIStalk Connect.




I’d be very careful here: ONC renews its Cooperative Agreement with DirectTrust
ONC’s work with DirecTrust is creating a cartel and will limit HIE choices and ultimately limit Direct or direct EHR to EHR interoperability across health systems and providers unless ONC dramatically changes it’s approach and creates affordable alternatives to Trust and Trust Bundles.
DirectTrust will quickly become the Medallion that Cab Drivers in San Francisco and other metro areas have to spend 250k + on simply to be allowed to drive a cab.
If we want to democratize data exchange, we MUST force ONC to simplify and streamline direct EHR to EHR exchanges and not allow any company to put road expensive toll booths on the road to exchange.
Athena’s set back this week with the OIG also ultimately hurts low cost exchange.
Look carefully at who’s really behind DirectTrust and you’ll understand who expects to make money there. These organizations want to force a middleman into exchange and require medallions that only these middlemen will be able to afford.
Although I can understand ONC’s DeSalvo’s desire to be less ‘siloed’ I think if they move aggressively in this direction it could be the death knell for best of breed vendors. Even in the 2014 and 2015 test criteria there are numerous data requirements that include data outside a specialty vendor’s focus area (such as why is cause of death in the demographic criteria?). I have no problems with setting up tests to see if there is ‘interoperability’ but at the same time they will need to allow for best of breed tools which they only reluctantly did as test criteria evolved over three years. If they do, not they will kill-off thousands of specialty vendors and millions of jobs.
When the test criteria came out in 2010 they were biased to single vendor solutions and still are…
TPD likes the Wall Street Journal site for CMS payments because if you leave the specialty blank, and just enter the city and state you’ll get the hospital and doctor payments for the location you have entered which will eliminate the need for entering each specialty separately.
As for the Heartbleed vulnerability, you can go to the Mashable website to determine what action you may or may not need to do for your website uses. Here’s the link to do so: http://mashable.com/2014/04/09/heartbleed-bug-websites-affected/?cid=146326&ctst=1
TPD!
What’s up with the audio playing over itself from multiple feeds on this site when click the link from the email? This only happens the first time I load it. If I refresh or click the link again, it won’t do it again.
[From Mr H] It doesn’t do that for me, although one other reader reported the same thing. There’s no audio embedded in HIStalk, so when the first reader reported it, I assumed he might have had adware. Let me know if you can figure it out.