We think that Medicine is a scientific discipline, and we believe it too, right? So what is a core tenet…
News 11/9/11
Top News
![]() A remarkably frank Institute of Medicine report commissioned by ONC, Health IT and Patient Safety: Building Safer Systems for Better Care, urges significant government intervention with regard to the safety of healthcare IT systems. It takes shots at both HIT vendors and HITECH incentives, saying in the preface,
A remarkably frank Institute of Medicine report commissioned by ONC, Health IT and Patient Safety: Building Safer Systems for Better Care, urges significant government intervention with regard to the safety of healthcare IT systems. It takes shots at both HIT vendors and HITECH incentives, saying in the preface,
Stories of patient injuries and deaths associated with health information technologies (health IT) frequently appear in the news, juxtaposed with stories of how health professionals are being provided monetary incentives to adopt the very products that may be causing harm.
On the committee were researchers, academics, and practicing physicians. Vendors were not represented, although John Glaser of Siemens was a reviewer. These are the most interesting points from my quick read of the report.
- The report recommends that ONC require all health IT vendors to publicly register their products with ONC, starting with certified EHRs.
- It urges HHS to eliminate non-disclosure and limited liability clauses in vendor contracts that discourage users from sharing patient safety-related software concerns.
- It suggests that reviews of software applications be published publicly.
- It recommends that HHS form a council to develop criteria for the safe use of information technology.
- It urges HHS to require software vendors to report IT-related patient safety harm or concerns to a central organization and also encourage users to voluntarily report to that organization as well.
- Software-related problem reports would be reviewed by a new group that would be the HIT equivalent of the National Transportation Safety Board. The report says FDA is not up the task since it’s an oversight body, AHRQ is too research-focused, CMS is mostly good at threatening the income streams of providers, ONC doesn’t have the expertise, and Joint Commission and related organizations are so dependent on income from special interests that they can’t be objective.
- It observes that “poor user interface design, poor workflow, and complex data interfaces are threats to patient safety” and “lack of system interoperability is a barrier to improving clinical decisions and patient safety” once you get beyond lab-related terminologies such as LOINC. Overall, it is quite critical of system usability and observes that vendors don’t have much incentive to make their products interoperable with those of their competitors.
- The report says that the industry has done a poor job of regulating itself with regard to patient safety and suggests turning the whole thing over to the FDA to regulate if the foot-dragging continues: “These and other recommendations would comprise the first stage for action, greatly advancing current understanding of the threats to patient safety. However, because the private sector has not taken substantive action on its own, the committee further recommends that HHS monitor and publicly report on the progress of health IT safety annually, beginning in 2012. If progress is not sufficient, HHS should direct the Food and Drug Administration (FDA) to exercise its authority to regulate health IT.”
Reader Comments
![]() From Pachelbel: “Re: Vince’s article on Epic. Cache’ is not proprietary to Epic as it is owned by InterSystems. It can be an extremely fast database if implemented properly. Ask QuadraMed or any of the hundreds of other HIS vendors that use it. I suspect your gripe is with the way Cache’ was implemented. No database works well if the data structure or queries are malformed. Full disclosure: I’m a Cache programmer who has seen the good, bad, and plenty of ugly implementations of Cache’.” Cache’ is one of few technologies developed for healthcare that was adopted by the financial industry for mission-critical applications, with organizations such as Credit Suisse, Ameritrade, and a couple of stock exchanges using it.
From Pachelbel: “Re: Vince’s article on Epic. Cache’ is not proprietary to Epic as it is owned by InterSystems. It can be an extremely fast database if implemented properly. Ask QuadraMed or any of the hundreds of other HIS vendors that use it. I suspect your gripe is with the way Cache’ was implemented. No database works well if the data structure or queries are malformed. Full disclosure: I’m a Cache programmer who has seen the good, bad, and plenty of ugly implementations of Cache’.” Cache’ is one of few technologies developed for healthcare that was adopted by the financial industry for mission-critical applications, with organizations such as Credit Suisse, Ameritrade, and a couple of stock exchanges using it.
![]() From SouperDooper: “Re: Vince’s article on Epic. I agree with the points made about the Epic way, rookie staff, and high costs. But to say that GE and McKesson have equal functionality is beyond ridiculous.”
From SouperDooper: “Re: Vince’s article on Epic. I agree with the points made about the Epic way, rookie staff, and high costs. But to say that GE and McKesson have equal functionality is beyond ridiculous.”
![]() From Astrid: “Re: Vince’s article on Epic. This feels like ‘nobody ever got fired for buying IBM.’ I know a hospital where the VP had Epic where he came from and wanted Epic there, so it was a total rip-and-replace without a business analysis or needs analysis. I understand that a strict implementation keeps clients from shooting themselves in the foot, but that usually speaks to their lack of business sense, discipline, and management ability. Having an implementation guided by people without healthcare experience and knowledge seems to guarantee rework later.”
From Astrid: “Re: Vince’s article on Epic. This feels like ‘nobody ever got fired for buying IBM.’ I know a hospital where the VP had Epic where he came from and wanted Epic there, so it was a total rip-and-replace without a business analysis or needs analysis. I understand that a strict implementation keeps clients from shooting themselves in the foot, but that usually speaks to their lack of business sense, discipline, and management ability. Having an implementation guided by people without healthcare experience and knowledge seems to guarantee rework later.”
![]() From Lorenzo’s Oil: “Re: Catholic Healthcare West. Hear they’ve scrapped their dual Cerner/Meditech strategy and are moving forward with Cerner system-wide after Meditech problems, with Cerner picking up about 20 sites once they’re done. I also heard Epic tried to jump into the fray, but CHW didn’t like the exorbitant price tag.” Unverified.
From Lorenzo’s Oil: “Re: Catholic Healthcare West. Hear they’ve scrapped their dual Cerner/Meditech strategy and are moving forward with Cerner system-wide after Meditech problems, with Cerner picking up about 20 sites once they’re done. I also heard Epic tried to jump into the fray, but CHW didn’t like the exorbitant price tag.” Unverified.
![]() From Unbiased Consulting Firm: “Re: Epic. They clearly have a huge lead in implementations over the last 24 months, but the talent pool is not available to support those implementations, nor does the application support this market advance. Meditech, Cerner, and Allscripts … there is much to do with marketing and creating awareness. If you purchase Epic, you need to be able to support and implement it successfully. Each of these applications are market leaders – do not be taken by the media. Make your choice, but consider all the factors.”
From Unbiased Consulting Firm: “Re: Epic. They clearly have a huge lead in implementations over the last 24 months, but the talent pool is not available to support those implementations, nor does the application support this market advance. Meditech, Cerner, and Allscripts … there is much to do with marketing and creating awareness. If you purchase Epic, you need to be able to support and implement it successfully. Each of these applications are market leaders – do not be taken by the media. Make your choice, but consider all the factors.”
Acquisitions, Funding, Business, and Stock
Grant Thornton, LLP acquires Computer Technology Health Associates’ Health Solutions division, including five military healthcare contracts and the staff supporting them.
HMS Holdings Corp. announces plans to buy RAC contractor HealthDataInsights for about $400 million. HMS expects HDI to contribute $85 million in revenue next year.
Days after the SEC releases new guidance on the matter, HCA revises its accounting for the recognition of income from HITECH incentive payments. Last week the SEC indicated that the “gain contingency” accounting model was the appropriate income recognition model for payments. Under this model, HCA will “recognize HITECH income when its hospitals have demonstrated MU and the cost report information for the full cost report year that will determine the final calculation of the HITECH payment that is available.” HCA expects to recognize HITECH income of $100 million to $130 million in Q4 and $190 million to $220 million for the full year.
San Diego-based Perminova, which offers SaaS-based applications for managing cardiac electrophysiologic labs and cardiovascular surgery, gets $7 million in venture funding. Its software is used by UC Sand Diego and Mount Sinai in New York.
Sales
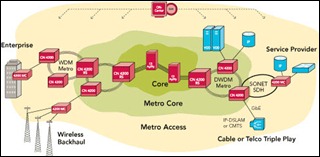
UC Health (OH) selects Ciena Corporation’s 4200 Advanced Services Platform to provide network connectivity across four hospital buildings and its data center facilities.
Iowa Health System chooses Jardogs’ FollowMy Health Universal Health Record to provide online access to its patients.
Conway Medical Center (SC) purchases PatientKeeper’s clinical suite of applications to automate physician workflow and drive physician adoption of HIT.
Kindred Healthcare signs for practice management and revenue cycle tools and services from MED3OOO.
People
IT service provider Systems Made Simple hires Viet Nguyen, MD as CMIO to advance technology initiatives to improve continuity of care and enhance patient safety. He was previously with KForce eGovernment Solutions and the VA Office of Information.
Optum’s Accountable Care Solutions team, led by Todd Cozzens, now includes over 700 cross-functional team members focused on aligning hospitals, physicians, and health plans for integrated care models.
Fast Company profiles Zynx Health Chief Nursing Officer Pat Button EdD, RN.
Announcements and Implementations
Cedars-Sinai Medical Center (CA) launches Voalte’s point-of-care communication solution following a year of research and testing.
Platte Valley Medical Center (CO) goes live on eCareNet, powered by Soarian Clinicals.
Rochester General Hospital (NY) and seven affiliated practices go live on Epic. They will spend $65 million over the next two years to convert the entire health system, which includes two hospitals and 40 practices.
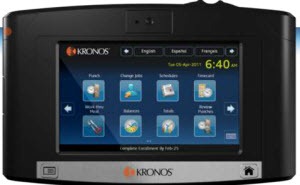
Kronos announces its InTouch time clock that features a color touch screen, gives employees access to their accrual balances and schedules, and supports off-peak use of apps such as employee surveys or streaming of informational videos.
Technology
Panasonic expands its Toughbook line of ruggedized laptops, popular in hospitals, to the Android-powered Toughpad, initially available in 2012 in a 10-inch form factor ($1,299) with a 7-inch version to follow.
Other
CCHIT announces that AOD Software’s Answers EHR and HealthMEDX Vision are the first EHRs to earn its Long Term and Post Acute Care certification.
Home health agencies, by the way, will see a 2.3% decline in Medicare payments next year under a newly released regulation. Opponents claim the cuts will leave half of Medicare home-health agencies operating in the red in 2012.
Community hospitals are progressing with their EMR implementations, with 69% saying they have acquired the technology and 39% of those reporting that their EHR project will cost over $8 million. The same report finds that almost all community hospitals have begun the conversion to ICD-10, though only a quarter are currently undergoing remediation. Forty-three percent of the hospitals say they are participating in HIEs.
The local paper provides an update on Cape Code Healthcare’s (MA) $20 million HIT investment, which includes a replacement of Meditech Magic with Siemens Soarian. Mr. H. interviewed Cape Cod VP/CIO Sheryl Crowley last year.
The HIMSS EHR Association announces its support of iHealth Alliance’s EHRevent, an online system for reporting adverse events. It’s part of the PDR Network, whose CEO Edward Fotsch MD was interviewed on HIStalk a year ago.
Eighty-three percent of clinical informaticists participating in a Billian’s HealthDATA survey report an improvement in quality outcomes from using EMRs.
CMIOs, CNOs, and senior nursing executives believe their roles and responsibilities will continue to evolve as new technologies are developed, according to a research report by Capsule. CMIOs indicate their most basic job function is to bridge the gap between clinical needs and IT, while CNOs and senior nursing execs see their roles evolving to be more inclusive of departments outside of nursing.
The EHR/HIE Interoperability Workgroup issues technical specifications to standardize connections between providers, HIEs, and other data-sharing partners.
Rival health systems HealthPartners and Allina Hospitals and Clinics (MN) claim their collaboration allowed them to shave $6 million in medical costs for patients across two counties. The organizations are participating in a seven-year “learning lab” that involves the pooling of resources, sharing of EMRs, and mining of insurance claims data for about 26,700 people with private insurance.
Kevin Lasser, CEO of JEMS Technology, compares Ford’s smart phone app for owners of the Focus Electric to his company’s own telemedicine app in My Ford Magazine, distributed to 4.7 million recipients.
![]() I featured Aventura in one of my Innovation Showcases and at least two readers have told me they’ve gone to work for the company. CEO Howard Diamond writes a post for Boulder Startups urging entrepreneurs to jump into healthcare IT: “The software and other tools that are supposed to be building efficiencies, reducing errors, and building collaboration and trust across caregivers are actually having the opposite effect; they are creating barriers to efficient quality care.” I like the list of information sources he provides for those interested in the healthcare revolution: Clayton Christensen (the Harvard professor who wrote The Innovator’s Dilemma), Regina Herzlinger (the Harvard professor who wrote Who Killed Health Care?), HIMSS (which needs no introduction), and HIStalk (the non-Harvard, non-professor known mostly for goofy music recommendations and HIT rumor-mongering.) Howard’s just being nice since I profiled his company.
I featured Aventura in one of my Innovation Showcases and at least two readers have told me they’ve gone to work for the company. CEO Howard Diamond writes a post for Boulder Startups urging entrepreneurs to jump into healthcare IT: “The software and other tools that are supposed to be building efficiencies, reducing errors, and building collaboration and trust across caregivers are actually having the opposite effect; they are creating barriers to efficient quality care.” I like the list of information sources he provides for those interested in the healthcare revolution: Clayton Christensen (the Harvard professor who wrote The Innovator’s Dilemma), Regina Herzlinger (the Harvard professor who wrote Who Killed Health Care?), HIMSS (which needs no introduction), and HIStalk (the non-Harvard, non-professor known mostly for goofy music recommendations and HIT rumor-mongering.) Howard’s just being nice since I profiled his company.
![]() I bet the Harvard people have more time after their day jobs to pursue their side ventures than I do, though. Mrs. HIStalk keenly observed this weekend that “whatever it is you do upstairs all the time won’t get done when you kick the bucket.” That’s the extent of her knowledge about HIStalk.
I bet the Harvard people have more time after their day jobs to pursue their side ventures than I do, though. Mrs. HIStalk keenly observed this weekend that “whatever it is you do upstairs all the time won’t get done when you kick the bucket.” That’s the extent of her knowledge about HIStalk.
New York’s state controller nixes a proposed $22 million deal with Allscripts that would have created a call center for SUNY Downstate Medical Center. Allscripts had reserved the right to send work offshore, raising confidentiality concerns.
Practice Fusion is named top EMR for ePrescribing and helping practices achieve Meaningful Use by Brown-Wilson’s Black Book Rankings.
![]() I’m not an attorney, but this ruling by Colorado’s Supreme Court seems to uphold a previous verdict that a man suing Kaiser for malpractice can’t claim physician-patient privilege in denying Kaiser’s lawyers access to his electronic medical records. He had a heart attack while taking a treadmill stress test and is suing Kaiser and one of its doctors, but didn’t want the defense to be able to study his medical records. A footnote in the ruling sounds like a HealthConnect (Epic) commercial: “Kaiser’s integrated electronic medical record is instantaneously accessible by any and all Kaiser healthcare providers and is a hallmark of the services Kaiser provides.”
I’m not an attorney, but this ruling by Colorado’s Supreme Court seems to uphold a previous verdict that a man suing Kaiser for malpractice can’t claim physician-patient privilege in denying Kaiser’s lawyers access to his electronic medical records. He had a heart attack while taking a treadmill stress test and is suing Kaiser and one of its doctors, but didn’t want the defense to be able to study his medical records. A footnote in the ruling sounds like a HealthConnect (Epic) commercial: “Kaiser’s integrated electronic medical record is instantaneously accessible by any and all Kaiser healthcare providers and is a hallmark of the services Kaiser provides.”
![]() Next month’s mHealth Summit has added as keynote speakers Surgeon General Regina Benjamin MD and HHS Secretary Kathleen Sebelius. HIStalk (in the form of HIStalk Mobile) is a media partner, so our own Travis Good, MD will be providing daily reports. He’s outstanding at understanding and explaining the business of mHealth, so he’ll provide both health and business perspectives. It’s December 5-7 at the Gaylord National Resort and Convention Center in the DC area. Full registration is $525, or $195 for federal government employees. I had a pretty good time there last year and the venue looks much better than last time, although I’d miss the proximity to the National Mall and all the fun sites and restaurants nearby.
Next month’s mHealth Summit has added as keynote speakers Surgeon General Regina Benjamin MD and HHS Secretary Kathleen Sebelius. HIStalk (in the form of HIStalk Mobile) is a media partner, so our own Travis Good, MD will be providing daily reports. He’s outstanding at understanding and explaining the business of mHealth, so he’ll provide both health and business perspectives. It’s December 5-7 at the Gaylord National Resort and Convention Center in the DC area. Full registration is $525, or $195 for federal government employees. I had a pretty good time there last year and the venue looks much better than last time, although I’d miss the proximity to the National Mall and all the fun sites and restaurants nearby.
Sponsor Updates
- Mike Marvin of CareTech Solutions and Kara Wingerter of Blessing Health Systems (IL) will present a case study on increasing revenue with online pre-orders and sales at this week’s Greystone.net Healthcare Internet Conference.
- OptumInsight launches additional capabilities for its Netwerkes EDI service, including integration with Epic PM Systems claim administration and clinical information workflows.
- GetWellNetwork appoints Wellford Dillard as CFO.
- Facilities of Vitalité Health Network (Canada) will go live next week with a pharmacy medication order management system connected to its Meditech system and powered by Perceptive Software’s ImageNow enterprise content management system.
- ICA releases a white paper entitled All Health Information Exchanges Are Not Created Equal.
- Mac McMillan, CEO of CynergisTek and chair of the HIMSS Privacy and Security Policy Task Force, will serve a panelist for Clearwater Compliance’s HIPAA-HITECH Blue Ribbon Panel webinar How to Prepare for HIPAA Audits.
- Tee Green, president and CEO of Greenway Medical, will host a November 15 webinar on future trends in healthcare.
- Beacon Partners receives Epic’s “Community Connect” certification.
- McKesson launches RelayHealth in Canada at the HealthAchieve 2011 Conference.
- University Medical Center of Princeton at Plainsboro (NJ) selects ProVation MD for its GI department’s documentation and coding.
- DST Health Solutions LLC announces an agreement with 3M Health Information Systems to integrate 3M’s ICD-10 Code Translation Tool with DST solutions.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg.














Re: the IOM/ONC report it seems to me that the IOM started with the wrong question. Question #1 posed should have been- ‘Are Health IT/EHR systems, when implemented appropriately, safer and better than the current paper system in most hospitals and MD offices; as opposed to the question that apparently was posed: ‘are EHRs safe.’
Heck, getting out of bed in the morning is dangerous- it just beats the alternative. Once question #1 HAD been answered, question #2 could have been tee’d up- ‘How can we make EHRs better?” But that ship has sailed and now they and we in Tidy-Bowl mode. The wrong question was asked so we’re dealing with what may be the right answer to the wrong question. And it will be hard to get the toothpaste back in the tube, worms back in the can, etc. on this one from an ONC/IOM standpoint- and yes the press will have a field day, those running for office will have more fodder and Republicans (no issue per se with Republicans BTW) who are pushing for less (not more) government regulation will have a field day with this set of recommendations.
A remarkably frank Institute of Medicine report commissioned by ONC…and a remarkably un-frank response to the report from Farzad: http://www.healthit.gov/buzz-blog/electronic-health-and-medical-records/patient-safety-healthit/
Anyone smell Congressional hearings?
Bravo, the IOM report, bravo!!! (If you can’t see, I’m giving it a standing ovation as I applaud.)
I’m guessing lots of users will appreciate it, lots of vendors will get their hackles raised, and lots of Tea Party peeps will abhor the thought of yet another government oversight body to oversee HIT software with the associated expenses and bureacratic layer.
One more oversight governmental body will do about as much good as one more kibbutzing group commenting on the chaos and waste in US Medicine.
If we want standardization and interoperability the way to do it is to start with a very limited vocabulary that is absolutely mandated across every system. Not a few hundred thousand SNOMED-CT terms; a thousand of the most important high-level ones identically mirrored in ICD-10. Not thousands of drugs; a few hundred of the most important ones identically mirrored across RxNorm, FDB, Medi-Span…Get the most important things standardized first and add Ainhum down the road.
If we want better software the way to do it is to get government certification hoops out of the way and simply provide broad recommendations which are exactly that: Recommendations. Electronic Ordering by Clinicians; Availability of all information relevant to a patient; Computerized Charting….The market will innovate and figure out how best to do it, and whether or not the software is mature enough to implement a recommendation.
We suffer from too much, and not too little, regulation and oversight.
@skeptic: If we suffer from too much, and not too little, regulation and oversight and there is zero regulation or oversight of health IT, then what do you propose?
The IOM panel was pretty clear about the status quo:
“The current state of safety and health IT is not acceptable; specific actions are required to improve the safety of health IT.”
The free market won’t solve quality and safety issues in healthcare IT or healthcare in general, because it’s not a free (or efficient) market. Consumers of goods, decision makers and payers are all screwed up, and misplaced incentives ensure that providers will continue to make decisions that increase revenue but don’t necessarily improve outcomes.
Finally, the matter of safety, ie the lack of it, pertaining to HIT devices has hit the HIT national stage.
Ed F should not be so biased if his PSO EHRevent is to be anything other than a shill safety group for the vendors and a facade for safety.
Actually, the report was commissioned by former ONC Chief Blumenthal in an effort to depreciate the role of the FDA, ie, to conclude it was not needed. Surorise surprise.
Too bad Ed F that the report shows that PSOs such as EHRevent are meaningfully useless. Did you report on the 2000 Rx errors in Providence RI hospitals?
And a shout out “HERO” and “COURAGEOUS” to Richard Cook, MD who dissented to the conclusions as reported in Appendix E.
To Dr. Fotcsh:
My opinion differs. I believe the IOM asked the correct questions.
The answer to your proposed question “‘Are Health IT/EHR systems, when implemented appropriately, safer and better than the current paper system in most hospitals and MD offices” is – nobody really knows. The IOM explicitly acknowledges this:
… “For example, the number of patients who receive the correct medication in hospitals increases when these hospitals implement well-planned, robust computerized prescribing mechanisms and use barcoding systems. But even in these instances, the ability to generalize the results across the health care system may be limited. For other products— including electronic health records, which are being employed with more and more frequency— some studies find improvements in patient safety, while other studies find no effect.
More worrisome, some case reports suggest that poorly designed health IT can create new hazards in the already complex delivery of care. Although the magnitude of the risk associated with health IT is not known, some examples illustrate the concerns. Dosing errors, failure to detect life-threatening illnesses, and delaying treatment due to poor human–computer interactions or loss of data have led to serious injury and death.”
The technology is experimental.
In my opinion, that invokes the medical adage “First, do no harm.” There exist protocols for human subjects experimentation. The health IT industry has exempted itself from those protocols.
My overall thoughts on the IOM report are at http://hcrenewal.blogspot.com/2011/11/iom-report-on-health-it-safety-nix-fda.html
Scot Silverstein, MD
Drexel University
We just ‘jumped ship’ on our vendor for not being able to deliver functionality, much of which were safety deficiencies, and just heard last week of another institution bailing oin the same vendor, for the same reasons. Vendors enjoy unprecedented, and illigitimate, immunity in these times, and some form of oversight and accountability needs to be in place! You hearing this ONC? The HITECH act is like a kindergarten teacher quickly ushering her little ones across an extremely busy five lane freeway ‘because we’ve got to get to the other side’. Whoa, partner, slow down! Look, we all want to get to the other side, but here, now, and quickly? Isn’t there a safer way?
But what if National EhrTraffic Safety grounds flights? Won’t EhrCraft purchasers be in a terrible predicament?
I am a reader of Dr. Fotsch’s EHRevent newsletter.
His comment indicates a bias that generates genuine concern about the EHRevent safety organization.
Based on the CEO’s comment, that oragznization seems incapable of an unfettered approach to complaints that are sent in.
This is all the more reason for the FDA to be in charge of regulating HIT devices immediately.
Vince, if you’re right in your assessment of Epic, it implies collusion with HIMSS and KLAS at an unprecedented level – solid rankings on satisfaction with surveys beyond IT / CIO types (KLAS) and as well with HIMSS Davies awards and Stage 7 – Epic accounted for 90+ % of all Stage 7 sites for some time now.
Maybe, just maybe, even at the risk of offending you or someone you love, Epic does at least an OK job helping people be more efficient and make care safer than the average bear.
Maybe it just works. And, maybe that’s a good thing these days.
And, a word of support for those epic Epic staff members (upper and lower case on purpose) who come to work or get on an airplane each day and help some of the nations most complicated organizations be successful! Congratulations for what you do to make healthcare better in this country. Your contribution matters and is making an important difference to an amazing number of patients across this country!
And Vince, if there were so many better alternatives out there, why don’t you write about them and how people could benefit from them.
Mr H talks about not allowing vendor shills to write for the Readers Write section. Maybe it’s time to not allow vendor rants in that section either. Make it a moving forward contribution, not something as lame as what was posted.
Whoppee! An IOM report on Health IT so this issue is now solved and behind us, just as it was with patient safety in 1999 after “To Err is Human” and provider quality in 2001 after “Crossing the Chasm”. Lucky we don’t have to deal with those issues any more….
Matthew Holt,
I share your concerns.
You left out the 2009 National Research Council report on health IT (link). Nothing came of it.
Interestingly, I do note from the NRC/NAS/IOM sites:
The National Research Council (NRC) functions under the auspices of the National Academy of Sciences (NAS), the National Academy of Engineering (NAE), and the Institute of Medicine (IOM).” … “The IOM is the health arm of the NAS.”
Apologies in advance for brevity and my planned lack of additional comments re: this thread as my 100+ unanswered emails and 100+ employees who count on me for a living take precedent over this interesting dialogue; but I have two brief items of note- one minor and one more major:
Minor- my comment re: the wrong question posed to the IOM re: EHRs was not meant to ruffle the foundational garments of any readers of this epistle but rather as a statement of the obvious (at least to practicing community based physicians where I spent a decade of my life), that a discussion of EHR safety per se was nowhere near as important as the decision that they face- ‘Should I adopt an EHR or not- and which has more liability and impact on patient safety.” Most practicing community-based physicians have little time left in their day for abstract musings, policy wonks or hapless banter, and simply want to know “Am I (and my liability) and my patients better off if I adopt and use and EHR or not?” ‘Pretty simple!
Major- EHRevent is a free service governed by a group of board members of the not-for-profit iHealth Alliance whose goal is to protect the interest of patients and providers as information technology is adopted in healthcare. They were founded a decade ago. My role, and that of PDR Network for whom I provide services as the CEO, is to provide pro bono network support for EHRevent. As to comments re: my allegiances; I apologize if our pro bono services are offensive to readers. As to impugning the integrity of the board members of the Alliance and the EHRevent service which they govern, I would note that many of them are senior executives from medical societies, patient safety groups and professional liability carriers whose existence and decades of experience focus on patient safety and provider liability. If you elect to challenge them on related issues- eat your Wheaties!
Back to work. ef