I'd never heard of Healwell before and took a look over their offerings. Has anyone used the products? Beyond the…
Monday Morning Update 8/30/10
From Packerbacker: “Re: Epic. Wins another one, selected VOC at Children’s Hospital of Wisconsin. The contract is not signed, but they have already started planning the implementation.” Unverified, but Epic doesn’t lose many deals in its home state.
From Winston Zeddemore: “Re: clinical data. I lost a lost of respect for Halamka with the whole ePatient Dave mess. As a doc, he should have known better than to inundate unsuspecting patients with a barrage of unchecked claims data in their PHR. Then, he has the audacity to state that the switch to ICD-10 would fix the problem, when ICD-10 has no code for metastasis of cancer to the skull, either. Recall, poor Dave was alarmed to see a diagnosis of mets to the brain, when he had really had mets to skull that had been successfully managed. Well, ICD-9-CM has no code for mets to the skull, so the coders used the closest thing, mets to the brain.”
From Telluride: “Re: HIStalk e-mail list. Since you started telling the numbers, it has grown each month. Do you allow unsubscribes?” Yes, and I get some of those. That’s why I look more at the ratio of new subscribers to unsubscribers. This month, for example, it has been 372:64. Some of those are e-mail address changes, of course. Like everybody else, I’d prefer readers who love me rather than hate me, but it’s indifference that I really hope to avoid.
From Eroica: “Re: Emdeon. I thought you’d like the highlighted reference below. You are now the source for Wall Street analysts!” A brokerage and investment firm’s update cites my Thursday posting about Emdeon and Blue Shield of California, although not by name (“a well read HCIT blog”). The announcement included the same confirmation I used from the reader’s rumor report (Blue Shield’s Web site) and listed the same three of 17 remaining clearinghouses that I did (which I did because those three are HIStalk sponsors and I figured it was nice to mention them, plus I hadn’t heard of most of the rest anyway). Emdeon responded to the firm’s inquiry by saying they may still negotiate a deal and their revenue from Blue Shield of California isn’t that important since “they can shift the cost per claim to providers or obtain rebates from other vendors.”
From Paul: “Re: tube system failure. Shameless plug by a robot vendor – I work for Aethon, a Pittsburgh-based company that makes TUGs, autonomous robots that deliver medications or supplies to any location. Think of it as a tubeless tube system with no fixed infrastructure that works 24/7. We also offer a Chain of Custody solution that uses biometrics and RFID to improve patient safety.” Since Paul made it clear it was a shameless plug, I’ll allow it. I’ve mentioned the company a few times, mostly when execs from other Pittsburgh-area HIT companies ended up there. Above is a video some guy made as he chased around one of the Aethon robots at El Camino Hospital. You’ll hear him say, “Puttin’ Americans out of work,” which may be true at El Camino since the hospital just announced a 140-employee layoff.
From C’mon Man: “Re: tube system at UPMC Shadyside. The workaround to avoid the >90 minute delay after CPOE deployment is marvelous!” CM sent a UPMC internal document describing a quality improvement project at Shadyside. Before Cerner was implemented, the ED stocked 95% of the meds they used in their automated dispensing cabinet and the other 5% were requested by tubing the paper order to pharmacy, resulting in a pretty good turnaround time of 28 minutes. With CPOE, the ED had no good way to alert pharmacy about those 5% of meds, so turnaround time shot up to over two hours. An ED nurse came up with a solution: tubing a yellow “Stat ED Med” card to pharmacy along with an index card listing the patient and med needed, dropping TAT back to six minutes. I was initially appalled at this solution since hand-transcribing an electronic order onto a tubed index card seems fraught with potential error, but pharmacy reviews the electronic order before sending the med and I assume nurses still verify the med electronically in the ED, hopefully with bar code checking. What puzzles me is why the original electronic order doesn’t go directly to pharmacy anyway — surely the pharmacy module should “know” that an order was entered for a non-Pyxis order and should send it to the pharmacist’s work queue for verification and delivery with no manual notification required. That’s what integrated systems are supposed to do.
All this tube system talk stirred up some old memories of a hospital I worked in years ago, where the information superhighway was a dumbwaiter system (“the dummy”, staff called it). It was actually darned useful since the hospital was built around it, so it connected the nursing units with the major departments they interacted with (lab, materials management, pharmacy, etc.) I once dared a small female co-worker to ride it up several floors, where she proceeded to scare the bejesus out of the nurse who opened its tiny door to see what had been sent. All of these “hospitals of the future” with their LCD TVs and room service should have reintroduced the dumbwaiter, an express elevator for stuff.
Listening: I’m still obsessed with the new Iron Maiden, but I took a break to listen to some catchy and refreshingly different alt rock-pop from The Last Goodnight.
Your mission, should you choose to accept it: (a) put your e-mail in the Subscribe to Updates box, just to make sure you don’t miss any news or juicy rumors; (b) speaking of news or juicy rumors, send me some by clicking the ugliest, greenest graphic on the page, to your right; (c) show HIStalk’s sponsors some appreciation by clicking on their ads to find out what’s new with them; (d) fritter away a slow afternoon at work by performing endless searches using the Search function to your right; and (e) Friend or Like Inga and me on Facebook so we can maintain our delusions of popularity. Thanks to readers for reading, sponsors for sponsing, and everyone who takes the time to leave a comment, send an e-mail, or submit something I can use on HIStalk, HIStalk Practice, or HIStalk Mobile.
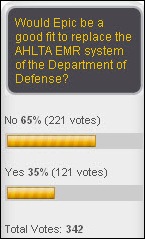
Epic wouldn’t be a good choice to replace the DoD’s AHLTA EMR system, two-thirds of HIStalk readers say. New poll to your right, since Ed Marx’s “Blessing of the Hands” piece stirred up some heated responses: should hospital IT people be expected to have a higher level of compassion and spiritual beliefs than their counterparts in banking or manufacturing?
A sad medication error at Cincinnati Children’s: a seven-month-old baby dies after heart surgery when a technician apparently infuses an alcohol solution instead of saline.
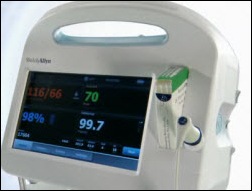
Welch Allyn announces its Connex vital signs documentation system, a single device that collects automatic instrument readings (heart rate, blood pressure, temperature, pulse oximetry) and manual entries (height, weight, pain level) and modifiers (body position, O2 settings). It also allows alarm management and on-screen documentation right from the device. It’s wireless to the bedside. The company says that an average 200-bed hospital wastes 8,000 hours per year documenting vitals and makes 10,000 mistakes in doing so. St. Joseph’s Hospital Health Center in Syracuse, NY, the beta site, reports a 50% drop in documentation time and 75% fewer errors.

Yale-New Haven Hospital’s new CIO will be Daniel Barchi, who will also serve as CIO for the Yale School of Medicine. I interviewed him a few weeks ago while he was SVP/CIO of Carilion Clinic of Roanoke, VA. YNHH will be cranking up its $250 million Epic project, so I’m sure his experience in implementing Epic at Carilion will be valuable. He’s a good guy, as was his now-retired YNHH CIO predecessor Mark Andersen. Both are fans of HIStalk and have been cordially forthright in responding when I’ve pestered them to verify reader rumors.
Also on Inc.’s list of 5000 fastest growing private companies: Vitalize Consulting Solutions, among the fewer than 10% of companies on the lists that have four-peated since the magazine started the list four years ago. I’d consider Vitalize CEO Bruce Cerullo to be a great friend of HIStalk, having known him for years and interviewed him in 2007 when he was running VCS’s predecessor company Lucida, but even I didn’t know the company had grown this much: 264 employees, $48 million in annual revenue, and three-year growth of 179%.
HIStalk reader and clinical informaticist Lincoln Farnum sent over his exclusive article, Common Knowledge: Clinical Decision Support in the Era of Meaningful Use, a CDS Toolkit. I’ve posted it on Drop.io, hopefully free of the sneaky and unwelcome Facebook tie-ins that keep biting me in the rear when I post files for download. It’s a good overview of CDS, the ethics involved in deploying it, the problems with trying to measure its impact on patient outcomes, usability issues, and best practices in CDS deployment. Give it a look.
I was annoyed by a press release from Brainware that announced a new healthcare customer without naming them (is a sales announcement really news when it omits the customer’s name?), but the company’s Distiller product still sounds kind of interesting. It’s an intelligent data capture platform that “learns” the data fields from scanned documents such as invoices and orders.
New from Japan, which seems obsessed with high-tech toilets: a network-enabled health monitor version that checks blood sugar, BP, BMI, and urinalysis, all stored for a year for a family of four. Plans for the next version of the $5,000 marvel include communicating the measurements directly to physicians. Maybe it can do its own health check and page a network engineer to bring a plunger.
Interesting: McKesson’s only obvious operation in Ireland produces software documentation (check the title page of your Horizon manuals), but McKesson books (no pun intended) $10 billion a year through its Irish subsidiaries. The reason: it routes drug sales revenues from Canada, Israel, and Mexico through Ireland to avoid the higher corporate income tax of other countries, like the one its $35-million-a-year CEO lives in. Blame the politicians, not the company — wasn’t that one of the many populist windmills that President Obama was going to joust at?
Two radiology department employees of St. Luke’s Hospital (FL) are arrested for stealing hospital computers and selling them on Craigslist. Funny that nobody at the hospital missed them until a tipster told them.
A review of computer records leads to a $5.3 million settlement between doctors and Central DuPage Hospital (IL) over a case of untreated clotting problems that may have caused a patient’s death. The radiologist said he never saw the patient’s MRI results, but the computer showed otherwise.





I am religious/spiritual myself, but your poll question is loaded. I say Yes for compassion, No to spiritual beliefs. A person may have either one without the other.
should hospital IT people be expected to have a higher level of compassion and spiritual beliefs than their counterparts in banking or manufacturing?
Ideally, yes – except when the manufacturing is of drugs or medical devices, the latter including health TI systems.
Almost all U.S. corporations with significant overseas revenues pull these kind of shenanigans though well structured off-shore affiliates. Reason why the effective tax rate of most U.S. corporations is incredibly low or even $0. Basically it is a shell-game. They hold it until there is a ‘tax-holiday’ with low/no penalties at low or no income tax rate.
Yeah the U.S. could slash corporate tax rates but unless it was 0% they should pull these kinds of shenanigans. Frankly, whenever I listen to a major corporate CEO or the US Chamber of Commerce tell me what America needs to do to ‘boost its competitiveness or create jobs’ I almost always know it is generally the opposite of those policies unless it is generic things like improve education levels in America.
I agree with Winston’s comment above regarding John Halamka. I was very surprised that Halamka did not make Modern Healthcare’s Top 100 Healthcare Executives. It has appeared to me for quite some time that Halamka was positioning himself to replace David Blumenthal when the ONC position wb available in the future. But it doesn’t look good with the ePatient Dave mess.
http://www.modernhealthcare.com/apps/pbcs.dll/gallery?Avis=CH&Dato=20100823&Kategori=PHOTO&Lopenr=823009999&Ref=PH
Re: Shadyside, With CPOE, the ED had no good way to alert pharmacy about those 5% of meds, so turnaround time shot up to over two hours. An ED nurse came up with a solution: tubing a yellow “Stat ED Med” card to pharmacy along with an index card listing the patient and med needed, dropping TAT back to six minutes.
From the medical informatics perspective, the lesson here is that the physician is no longer the “learned intermediary” between computer and patient.
This model from the earlier days of simple advice-and-records keeping health IT no longer holds:
[Computer] [Clinician] [Patient]
Rather, the computer has become a cybernetic governor of care, as in a programmatic intermediary between clinician and patient regulating care operations:
[Clinician] [Computer] —> [Patient]
The fact that a “workaround” a.k.a. “override around cybernetic regulator of care” had to be created in order for appropriate care to be delivered in a critical care environment supports the latter conceptual and legal model.
Many thanks for the link to the interesting and informative article on CDS by Lincoln Farnum: “Common Knowledge: Clinical Decision Support in the Era of Meaningful Use, a CDS Toolkit”.
Under the chapter on “Practical considerations for the development of CDS” I would like to add to the “Monitor impact, get feedback, and respond” paragraph – the capability of a CDS to close the knowledge loop, in the form a machine learning mechanism:
The CDS is offering an “expected” advice (e.g. differential diagnosis or therapeutic consideration).
Reality will provide an “observed” fact (e.g. true diagnosis, therapeutic outcome) as a feedback to the CDS algorithm.
Once a CDS has given a certain “expected” advice, it should be capable of learning from reality, from humans’ experience, from a patients outcomes’ database – what is the real “observed” diagnosis, therapeutic outcome. This information should be available in databases (EHR are supposed to create) and the methodology for fine tuning machine algorithms with “observed” knowledge feedback, while not easy nor obvious, are still doable.
I like the Welch Allyn device but really now: “The company says that an average 200-bed hospital wastes 8,000 hours per year documenting vitals and makes 10,000 mistakes in doing so.”
10,000 mistakes on vital signs? Are you kidding me? Where is that published?
And who is validating the accuracy of the machine? Does it work this way?: If the machine reports the BP is 231/74 and it gets silently entered in to the record, who knows, and can you trust the machine? Will hydalazine be mindlessly given, only to find out that the BP was really 110/83?
Where does the FDA enter the picture on regulating the device, the interfaces, and the digital siloing of the results?
There is already too much “out of sight, out of mind” adversely affecting care.
This would appear to be another impediment to the bedside care and nursing assessment of the sick patient.
BlueDog,
I too was surprised that John Halamka did not make Modern Healthcare’s Top 100 Executives. However, this is a reader’s survey. Knowing that year after year the HIMSS staff, BOD, and members were pressured by Executive Staff to vote for H. Stephan Lieber, I do not hold that listing in high regard. We all wanted our bonuses, so we did whatever it takes to guarantee them.
Mr. Histalk’s blog is a much better gage of the overall HIT industry than Modern Healthcare, whose choices for top healthcare executives have always been questionable, considering Lieber has made that list each year.
I was surprised not only that Senator Grassley made the list, but that he was listed before David Blumenthal MD.
Alcohol v saline: Baby dies “when a technician apparently infuses an alcohol solution instead of saline.” Isn’t this the hospital visited by HHS Secretary Sebelius, who heaped praise on its modernity? You covered this, Mr. HIStalk, a few months ago, I think.
A similar incident in Cleveland’s Rainbow landed a pharmacist, Eric Cropp, in jail, when on a Sunday morning, the pharmacy IT system was suddenly not working, staff was over worked, a technician was on the internet, and medications were prepared in error.
The coverage on this case misses any investigative aspect. There is a difference between alcohol and saline, right. Were they lableled incorrectly, were the techs doing workarounds with tube systems, were there distractions caused by too much moedernity with electrical workflow IT systems?
Mr. HIStalk, please try to find out. The world of medical care needs another lesson learned. Thanks.
Interesting on the Welch-Allyn product – it looks like a mini-EHR – CIS. Will they be getting it certified to the ONC meaningful use criteria (stage one specifies electronic charting of height, weight and blood pressure)? Or are they going to position it as a ‘displayable middle-ware app?’ Actually, that brings up an interesting question – does one have to provide all of the functionality described in the ONC MU criteria or just some parts of it to be certified? What if a doctor’s office uses this Welch-Allyn product and some other specific product for the other functionality required for MU – would it have to be all integrated or would the modular aspects of it be OK for the $$$$?
Take a listen to the Sensational Alex Harvey Band ( if you can find it)
Please consider a poll/survey (draft below):
To single practice docs- what are your monthly EMR payments?
a) $1000 /month
Great comment by A. Scarlat MD. That’s when CDS will become truly useful.
Re : poll question.
I agree with vendorinsider. It’s a badly worded poll that will skew results.
“Should hospital IT people be expected to have a higher level of compassion and spiritual beliefs than their counterparts in banking or manufacturing?”
Apart from the compassion/beliefs not being mutually exclusive part, even your average thief has higher compassion than somebody in banking. They tend not to steal from their own 🙂
Just in general I see people taking these polls seriously. Apart from the wording issues, on-line polls are always self selecting and really aren’t anything more than a little fun.
Alcohol vs saline – alas, reminds me of a patient in the VA over 30 years ago…an alcohol based product was injected into his brain instead of a dye solution. Hospital staff were shaken for years afterwards.
Feel like I’m in a time warp today reading the comments on Halamka and ePatient Dave. That was brought to the attention of the popular media quite some time ago, Halamka readily admitted it was a problem and he and others are trying to figure out what might be a better approach for sharing PHI with citizens in the future.
This is not an easy problem to resolve and it will take time to address both technical and policy issues.
to John@chilmark. The problems were easy to anticipate and should have been addressed PRIOR to implementation, not the other way around. Admitting problems you should have known about beforehand doesn’t buy you anything.