Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…
News 1/6/10
From HIPPAcrates: “Re: notice of proposed rule-making. The summary spreadsheet is very useful, thanks. I just found this error in the government document and hope it’s not an omen.” Even the feds can’t spell HIPAA with the full wording right in front of them. Surely I’m not the only one who knows how to modify Word’s dictionary to catch gaffes like this.
From Dean: “Re: MU. Was just reviewing your summary of the meaningful use doc. Very nice work, even better than Halamka’s at geekdoctor, of course you probably don’t have a Kevlar suit or a handy folding bike! I think a great reader poll would be to ask whether people with CPOE installed have implemented drug-drug or drug-allergy interactions. My bet is that most people who have tried this have turned it off. I think this is a terrible requirement. Current drug-drug interaction checkers are way too sensitive and generate way too many false positives. I’ve reviewed some papers that reported over 25% of medication orders generated alerts. That is unacceptable in my book.” Maybe he needs the Kevlar suit because of bike-induced thigh chafing. The problems with clinical warnings are:
- Practitioners universally believe they don’t personally need them, but they think they should be turned on for their less-capable peers.
- Duplicate drug checking throws out a ton of false alarms and is useless 99% of the time.
- Allergies are often entered without the type, severity, and onset of the reaction, meaning that everybody’s “makes my stomach hurt” allergies trigger the Cry Wolf syndrome and allergy warnings are overridden 95% of the time.
- Users aren’t always given the tools to modify the warnings to suit their needs, such as expanding the by-the-book dose ranges and setting their own ranges based on experience.
- The few vendors of clinical data rigidly adhere to conservative manufacturer data and the advice of their overly cautious lawyers in overweighting accuracy at the expense of usefulness.
- Systems don’t allow personalizing the alerts, so while the family doc might benefit from a renal warning for a particular drug, it’s a sure bet that the nephrologist who gets the exact same warning surely won’t.
- Of all these, the last one could be easily implemented, other than the fact that data vendors, hospitals, and IT people don’t trust their docs to turn off warnings that they don’t value (a rather condescending “computer knows best” outlook).
From Crumbgirl: “Re: GE Centricity Enterprise. You will hear big news out of Indiana if you have not already!” I haven’t heard anything so far.
From Infodoc: “Re: your MU summary. Thought you’d like to know that the Advisory Board referenced your Meaningful Use summary in their Meaningful Use briefing published Monday. HIStalk is becoming a good example of a disruptive technology.” Honestly, all it took was a couple of hours of skimming the documents to pick out the relevant parts. I think the trick is that, as a nerd, I was the only pseudo-journalist sitting home with nothing better to do right before New Year’s. I do appreciate the nice comments about it, though. And I do like to disrupt whenever possible.
From Bob in Accounting: “Re: Epic’s newsletter list for customers to prepare for meaningful use.” My 99% condensed summary of what it said: (a) upgrade; (b) finish rollouts; (c) implement e-prescribing; (d) install MyChart; and (e) install Care Everywhere for data sharing.
From Chris: “Re: EHR. First off, I really appreciate your ongoing coverage of all things health IT related. As I’ve been reading your site and others, I’m failing to identify a distinction between EMR and EHR in terms of the ARRA/HITECH legislation, ‘meaningful use’ and certification criteria. Is there a true distinction between the two? I feel as though I see them used almost interchangeably. Thank you for your insights and clarification!” Theoretically, HITECH applies only to EHRs since the products must be certified and, by definition, all certified EMRs are actually EHRs since they are interoperable. I have a philosophical disagreement with that loose terminology, however, probably because vendors have latched onto it for marketing purposes for the same old products that pre-dated the EHR term. EMRs are used to treat patients. EHRs are used to manage health and community wellness, including collecting data from a much wider net than just doctors and hospitals. I’ll stand by my crotchety proclamation: I don’t care what vendors say, none of them have an EHR. That’s why I always call them EMRs unless I’m quoting someone else.
From Lacey Underall: “Re: Humana. A dermatologist takes them to small claims court. Way to go!” I love this. A dermatologist, tired of Humana not paying his claims for years ($120K total) but unwilling to pay a lawyer 40% to go after them, takes the insurer to small claims court by bundling the claims into packages that fall within the $5,000 limit. Humana’s lawyer is surprised, given that he has never been to small claims court. The doctor tells him, “This is the first of 25 claims we’ll be submitting … Humana could save those $350 filing fees times 25 and his time and fees times 25 if they would just process our claims." Even though the tactic hasn’t worked for other doctors because Humana got their case moved to federal court, it did this time: Humana coughed up $80K and the doctor is hoping to collect the rest of what they owe him before their next court date.
I’ll be charitable in characterizing the post-holiday response to my HISsies nominations plea as modest. The voting that will follow next week or so is going to be pretty dull if nobody nominates their best and worst vendor, industry figure of the year, etc. It takes just a minute or two and validates my pathetic existence, so humor me.
Former Cerner sales VP Mike Supple joins recruiting firm B.E. Smith as SVP of business development.
Ten-provider Orthopaedic Center of Southern Illinois chooses the SRSsoft EMR after its free trial, saying the docs are saving 30-60 minutes each per day.
Madrigal sent me an e-mail announcing Meditech’s merging of PtCT into its regular organization, which I reported last week. The company has posted the announcement and a company Q&A.
Universal Health Services chooses Cerner and its Remote Hosting Option for its 24 hospitals. The modules weren’t stated (red flag – did they commit to all of Millennium or just a few modules?), but per FlimFlam Man, they will replace Opus Healthcare, Siemens pharmacy and ADT, RMS, and others.
Cerner also announces a deal in which Tenet will increase its Millennium use from 14 hospitals to 47. Shares were up 6% today, hitting a 52-week high and raising the market cap to $7.29 billion and nearly making Neal Patterson a hemi-billionaire (he’s got $496 million worth).
Revenue cycle vendor Passport Health Communications names David Whitt CFO.
Jobs: Eclipsys Systems Engineers/DBAs, Anesthesia Product Specialist, Clinical Implementation Specialist.
Former Eclipsys SVP Tom Dunn joins QuadraMed as SVP of sales and marketing.
Tennessee gets $2.7 million in stimulus money for a project that CMS says will improve patient outcomes. Reading further: the money will be spent on “planning activities”, like doing a study to figure out why doctors won’t use EMRs.
Three Montana provider organizations go live on the beta version of EMix, a vendor-neutral cloud computing platform from DR Systems for sharing radiology images and reports. They claim it’s as easy to use as e-mail. The company pitches charging patients to manage their images online, for which it takes a cut of the revenue.
Newham University Hospital NHS Trust says its Cerner system is saving it money and reduced patient wait times. Patients in the same area are using Philips home monitoring diagnostic equipment in a test for NHS.
The owners of paging and communications systems vendor Amcom Software sell controlling interest to a partnership of a private equity firm and a venture capital firm. The private equity firm says they’ll probably sell it at some point.
I think I missed this when it was announced: Epocrates names Geoffrey Rutledge MD PhD, formerly of Wellsphere, as CMO/EVP of product development.
Google announces its Nexus One Android-powered cell phone. It seems anti-climactic, hardly an iPhone-killer. Too bad it didn’t involve cheap cell service, although maybe the master plan is to serve up phone ads that offer a lower cost all around.
Odd lawsuit: a woman sues Walgreens, claiming that a store employee leaving the bathroom knocked her down with the door. She wants medical costs, damages and “other sums to compensate her for her injuries,” claiming that Walgreens should have instructed employees to look before opening the door, for failing to tell her to move, and for failing to equip the door with a warning device.
HERtalk by Inga
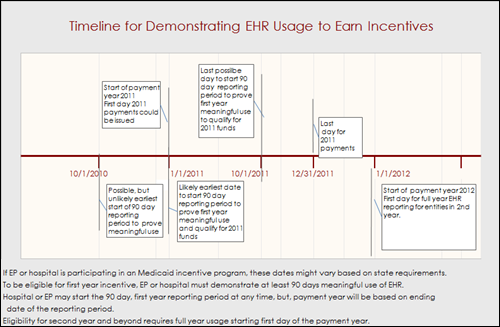
In yesterday’s HIStalk Practice, I touched on a few nuggets of information about the latest EHR meaningful use recommendations. I might add it is worth a read because there are some points Mr. H and I haven’t seen covered elsewhere (and while you are there, sign up for the e-mail updates.) One particularly confusing item relates to the timeline for proving meaningful EHR use in order to earn incentive dollars. I tried to summarize a bit on the timeline for getting money, but because it is particularly confusing, I decided a graphic might help (click it to enlarge).
For those that want to follow along at home, this information is found around pages 23 to 31 in the larger, 557-page document. As I interpret things, to qualify for stimulus money during 2011, a hospital or eligible professional (EP) must demonstrate meaningful use of EHR for “any 90-day period within the first payment year.” The earliest possible start date for that 90-day reporting reporting will likely be January 1, 2011. The latest day to start a 90-day reporting period and still qualify for 2011 money is October 1, 2011. After earning incentive money in the first year, entities will be required to prove meaningful EHR use for a full year, starting on January 1, in order to qualify for second-year funds. Thus, if an entity qualified any time during 2011, it would have to continue to prove that it used its EHR meaningfully from January 1, 2012 to December 31, 2012 in order to qualify for the 2012 incentive funds. And, if the entity doesn’t try to qualify for the first time until sometime in 2012, then it must prove meaningful use for the full year beginning January 1, 2013, to get the second-year funds. And so forth. If someone interpreted things differently (or can explain this better), please advise.
athenahealth signs a deal with Caritas Christi Health Care to offer athenaclinicals to 500 employed providers and 1,200 affiliates. CIO Todd Rothenhaus, MD, the Caritas SVP/CIO, confirmed to me that Caritas will offer athena and eClinicalWorks, which was announced previously.
I was talking EMRs with a girlfriend at lunch today (isn’t that what most gal pals do?) and we agreed that we can’t think of any providers that currently enter 80% of their orders themselves. We thought we might come up with a doctor who uses e-prescribing 75% of the time (but we thought of lots of reasons why a patient and provider might prefer the paper prescription). We couldn’t come up with a single small office group that is currently capable of sending patient data electronically to other providers (often times because the receiver can’t accept the data). The one bright spot is that the recommendations clearly state that “documenting a progress note for each encounter” is not a requirement for proving meaningful use. Otherwise, the mountain is high.
Ridiculously sad, any way you look at it. An unemployed, unmarried 35-year-old mother of nine sues three doctors and two nurses after being sterilized against her will. The mom was delivering baby number nine via a planned C-section and and asked for an IUD to be implanted immediately after delivery. Instead, the doctors performed a tubal ligation.
Trinity Health (MI) buys 1,200 bundled EHR/EPM software licenses from NextGen, increasing its rollout to all employed providers in its network.
Happy 2010, by the way. The ever-generous Mr. H gave me a bit of time off during the holidays, but now I am back at it. Mr. H and I have each waded through pieces of the latest meaningful use documents in hopes of becoming industry experts. Unfortunately, at least in my case, more wading is required. I was hoping there might be some clarification about what exactly a “certified EHR technology” is. Of course “CCHIT” is never mentioned anywhere, even though it seems a given that CCHIT will be a requirement since they are the only certifying body out there. Why can’t the Secretary or the ONC come right out and say it’s CCHIT 200x for now? That way buyers know what is required and vendors know what they need to do if they want to participate.









I know of quite a few places that have very strict operational policies on CPOE and thus have very high CPOE compliance/%, better than 80%.
On the topic of med alerts, that is so true about all of them not wanting the alerts for themselves, but thinking they’re great for the less skilled of the bunch.
I have yet to meet a Dr who has not learned from the drug warnings and the drug education summaries. Many don’t admit it to their colleagues. The never admit are the ones I never recommend to my friends.
The best MD’s I know after working with thousands of them… are often very eager to leran more, and realize no one knows it all. They accept new knowledge from their EMR drug warnings etc… and share that information with associates.
EMR Dude,
Thanks for informing us about the educational preferences of good physicians. So kind of you.
Allow me to return the favor:
The best IT personnel I know are often very eager to leran more, and realize no one knows it all.
Those seem unfortunately uncommon in HIT today. In fact, the situation is perhaps worse than we think. See my post at http://hcrenewal.blogspot.com/2010/01/more-on-perversity-in-hit-world.html
Decision Support: The EMR Dude and CPOE Fan have never been forced to use this nonsense that warns of trivial interraction incessantly but ignores a dangerously high dose of medication from a mis-click. Has said decision support devices been approved by the FDA? Whose decisions are being supported? Whose judgment is interfering with my staff’s work?
Problems with decision support should be reported to the health departments and any other body that comes to mind. We have faound the mistakes time consuming and risky.
MU summary: I agree with all the other posters that it has been very useful. I stole it and made it into a powerpoint for use with my executive team.
Is it plagiarism if I tell you I did it?
Inga –
I like your timeline. One thing to note is that for Medicaid meaningful use in the first year has a different standard of success. In the first year for Medicaid you only have to begin “adopting, implementing or upgrading certified EHR technology”. This applies to both EPs and hospitals.
Has Tenet signed a do not disclose contract?
It seems Socky the HIT Sockpuppet a.k.a. “Programmer” a.k.a. “IT Guy” at blogger/HC Renewal has disappeared since my little forensic exercise inked above in my January 6th, 2010 at 10:09 am comment.
That HIT company-based trolls would resort to psyops to support diffusion of tools that are eliciting widespread complaints from physicians — about the tool’s interferences with patient care, in fact — is perverse, whether company-sanctioned or not.