Aasim Saeed, MD, MPA is founder and CEO of Amenities Health of Dallas, TX.

Tell me about yourself and the company.
I’m a Texas native and I live in Dallas. I have a medicine and public policy degree background, but I never practiced clinically after medical school. Instead, I went the route of management consulting at McKinsey, where I was almost exclusively focused on US healthcare and US healthcare systems specifically. I wanted to make an impact on the healthcare provider side. That remains my passion today. I was at McKinsey for a few years and then started getting into technology and jumped out from my first startup, which was an early stage fintech company that was acquired by H&R Block.
For the last four years, prior to launching Amenities about two years ago, I led innovation at a large healthcare system here in Dallas, Baylor Scott & White Health. It was an interesting time to be there from 2017 to 2021, when I left. Obviously COVID happened, but we also made massive investments in digital health, and I think we were pretty much leaders in the field from a health system side. That has a loaded connotation onto itself, but I did a lot of cool things, part of which sparked the ideas and opportunities that I wanted to explore at Amenities.
At Amenities, we help large healthcare systems build a much better patient experience. Specifically, we think that the digital consumer is dramatically lacking in US healthcare, and that health systems have a huge opportunity to shift the market experience and then hopefully get rewarded for doing so by moving patient volume.
We call our platform a digital front door and patient loyalty platform. That last part is important, because our bet is that if you not only improve patient experience, but do so in a new business model that rewards you with loyalty, that could be game changing. That’s the idea behind Amazon Prime, where you went from occasionally shopping online to basically shopping online exclusively. I have hardly set foot in a Walmart again because two-day shipping and free returns solved all my concerns.
Part of what we are trying to do is help health systems figure out how to be more compelling and exciting to their patients. That’s why we’re called Amenities, literally.
Healthcare consumers have a high lifetime value. Why don’t providers compete on customer experience?
I don’t think there’s a single answer, if I’m being blunt, and I’m definitely not the smartest person in the room to have a perfect answer for you. They don’t compete on it because nothing changes your decision-making as a patient. If you’re in an ambulance, you’re not typically choosing where you’re going. If your doctor says go to Baylor, THR, or Medical City, you follow those instructions. You only find out what it costs afterwards. You are picking based on a vague idea – what’s a good doctor or good health system? There is an abundance of reasons that patients aren’t able to discriminate health systems.
If you’re being fair and say, why aren’t health systems more motivated? It is because to date, if they have done something, it hasn’t resulted in more volume. They might have experimented with doing something for the patient, but it didn’t move enough volume in a specialty that mattered financially. There is a massive missing ingredient, which is a business model that rewards them in a metric they care about. I think that is membership, loyalty, and lifetime value of a patient, instead of just saying that we offer this concierge primary care practice, we signed up 100 patients, and that’s it. It doesn’t result in downstream loyalty.
Patients want to know what it’s going to cost. I spent four years at Baylor trying to figure out how to do meaningful price transparency. Frankly, it’s not really a solvable problem right now, based on the infrastructure we have and the multitude of players.
There have been both handicaps for health systems, as well as that they haven’t had a financial business model that gets them excited enough about doing game-changing things. It’s sometimes unfair, but I think accurate, to say that this industry is known for conservatism. They don’t take big risks. They don’t swing for the fences. They don’t do this. We are trying to show them an opportunity not to do things for incremental cost reduction or try to find a use case for AI for AI’s sake, but rather let’s swing for the fences and change how healthcare is delivered here. Incentives around a membership could be a big activator.
Do health systems that launch innovation and digital teams have specific ideas of what they want to accomplish and establish metrics to track results?
You will find, unfortunately, some variation of the Triple or Quadruple Aim as the mission, just reworded to sound fancier, like reduce cost, improve quality, provider satisfaction, patient experience. At Baylor, when I was there but I think it’s changed now, we had value-based care. We had operational excellence. There was cost reduction. We had consumer digital, which was patient experience.
Again, they might call it something different, but we haven’t seen much that’s materially different than that in different innovation teams. That’s because we haven’t accomplished those goals. That’s not a knock on health systems. Those are the things that we are all trying to achieve.
The question is, how is it going to scale? Where health system innovation teams struggle is that everything feels like an experiment, with death by pilot or a dozen little pet projects. We very much started out that way. You have to get to the core of the health system and what’s it trying to do. You can’t experiment for experiment’s sake.
Unfortunately, we’re seeing a lot of that. We get asked a lot, what’s your AI strategy? What are you talking about? That’s such a weird thing in healthcare. It’s like, what’s your cloud? I mean, I understand why people care in the IT arena, but that’s not a business case. If McKinsey taught me anything, it was to start with a tangible outcome that is undeniably important to the overall business, and let your strategy, especially your technology strategy, stem from that.
The time that we had the most clarity at Baylor, and the digital health office that I ran, was during COVID. It was like, oh my God, patients can’t access virtual appointments and we’re not serving our patients. There was immediacy. But even immediately after that, our strategy became specific, to double the number of Texans served. That was so helpful for the innovation team to focus. We stopped doing things that just came to us, and we said, is this going to move the needle?
That’s a level of focus that I left with for Amenities, to say that we’re not an app for app’s sake. Building a prettier app is not going to fix healthcare. If the app helps a patient register in under 30 seconds, find a doctor, and book an appointment, now we’ve done something. If AI can help, great, but 90% of those problems do not require AI. We have refused to create the operational systems, the scheduling systems, or whatever it is. We fix those things. We don’t try to do big, shiny things. We’re trying to help the health system attract new patients, make it incredibly simple for them to become a patient, find a doctor, and book an appointment.
The fun really starts when we think, what would keep them loyal that doesn’t exist in the market today? When we think about loyalty, you have to be better than One Medical. You have to be better than than what’s out there in virtual health like Teladoc or whatever they can find on the street. There are creative opportunities to do new services that patients don’t know to ask for, but that they really love, based on our research.
What is the current and future state of the digital front door and patient portals?
For me, it’s absolutely clear. If your digital front door doesn’t add new patients simply and immediately, what is the point? That’s where patient portals are good. It’s good to have a patient portal, but they are completely lacking in imagination of what a comprehensive consumer experience should look like.
Starbucks doesn’t say, I would just like an app to review my history of orders. It is a transaction tool. Starbucks would never in a million years go to the Coffee.com app with Joe’s and Pete’s and everybody else all using the same app, that’s no big deal. Like it or not, health systems are competing. The fact that they defer their most valuable digital asset to another company is just beyond me. It is an acquisition tool. That’s what it is. That’s what it should be. The fact that it’s not viewed that way is a gross oversight, full stop. Are people getting into your system and are you adding new users? If not, then it’s lacking in what it could be, and how it could be financially ROI-backed in all of your investment.
At Baylor Scott & White, during COVID for 2020 through 2022, we added half a million net new patients through the app. That number for most other health systems, nine out of 10 of them, is zero. That’s crazy. That’s like health systems just now realizing that they need a website. That’s the equivalent of the app. In five or 10 years, we’ll look back and be like, that was crazy. Why would we limit use of the app to current patients or current customers?
I don’t know how that happened or why, but it’s a lack of imagination to say, this is a digital commerce acquisition and loyalty play. Once we earn a place on their phone, what are we doing to keep them using that? Why do they love that? Why are they coming back to us over and over again? That’s how every other business thinks. I don’t know why healthcare doesn’t think that way.
A simple healthcare problem is that someone can’t get in the app unless they are already a patient. We found that nine out of 10 people threw their hands up and said, “I guess I can’t get into the app.” Why can’t they register? Oh, we don’t want to create duplicate accounts. OK, great, then we need to ID verify them. How do you do that? There are only really crappy systems where you have to take a picture of your ID and wait for HIM to review it. We said no, we want to automate all of that, and that’s what we do. In 30 seconds, we can full ID verify someone better than literally Experian can, with no data entry required.
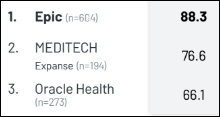
We don’t create any duplicate accounts. If they don’t have an account already, we register them into Epic in MyChart. We don’t have to make these sacrifices. The tech can do this. You just have to build an experience. Start with the experience that you are trying to create and then get it there. We got the idea from fintech and built that experience. The other one is airlines, which are the king of loyalty programs. No airline would ever say, here’s our loyalty program app, and you have to download this other Sabre app to actually book flights. That’s where health systems are. They haven’t forced these things to be the same. They haven’t said, “This is our brand and this is how we interact with everyone.”
Lack of transparency on pricing from a patient standpoint is a massive problem. I spent four years trying to figure out how to create meaningful price transparency for consumers at Baylor Scott & White, and two things went wrong. One is after like four years, we could tell them if their co-pay was going be $20 or $25. No one cares about that. That’s not the thing that they are worried about. They are worried about bankruptcy. They are worried about a surprise bill. Somebody’s out of network. The doctor who is wearing your scrubs, who has your ID badge, who is located inside your building, somehow doesn’t work for you. That’s the surprise.
We tested this and came up with a feature called no surprise billing guarantee. It was the number one feature wherever we tested. It’s an example of a feature that consumers aren’t asking for, but when you test it and you put it in front of them, it goes off the charts. The No Surprises Act exists, but patients aren’t understanding that, so let’s build a product around no surprise billing guarantee. That’s one of the primary things that Amenities does.
Health systems struggle to show their true pricing everywhere within a system. Baylor would direct you towards ambulatory surgery centers and not the main hospitals, because we all know that the pricing is cheaper for the same procedure at an ASC, but health systems aren’t really incentivized to do that. There was always this internal struggle. But I believe that health systems should embrace that and say, get on the patient side. Get on the consumer side. Because once you become a consumer advocate like that, that’s how you think big, not playing these games of, is that good for our hospitals, and what will that hospital president think? My push is to be on the consumer side completely.
Customers like to feel that the business knows them. Health systems people can look in the EHR for your medical history, but do they use technology as customer relationship management way to accommodate preferences or non-medical lifestyle information?
I was there when we brought in Dynamics and evaluated Salesforce as a CRM. CRMs are fine and definitely a tool, like cloud, that any modern company and architecture should be built on. It always comes down to, have we started with a use case? I see so many health systems, including ours, saying that we can’t do anything until we have a modern CRM that connects the website to the contact center and to our data. That’s just not true. That will take like four years, and if you don’t start with the use case, you won’t have the funding by the end of it. Everybody would be like, why did we just spend $50 million to do this thing and nothing has changed on our website?
You have to start with the basics. Can we register a new user? OK, great, and then to your point about preferences, what are all the different communications channels that they get, and how are we letting them set those preferences so that they are not getting a bunch of phone calls when they only want texts or other things? There’s a lot of little, immediate things. What often happens in healthcare is that once you start talking about CRM and big legacy platforms, it becomes a five-year journey, and you don’t know if you’ll make it with the same team by the end of it.
Amenities is keen to say, you can try to build what we built, but Baylor Scott & White spent north of $25 million trying to build the MyBSWHealth app. It was wildly successful, even at that number, but that’s insane. Why is every health system doing this? Part of why we left to do this is that we built this at scale. We can be live in a matter of weeks, if not months, whereas we’ve never seen a health system spend less than $5 million a year and take two to five years to build something custom. Why would you do that? It’s not a good idea. We have to do something with the health system industry experts, like what we’re trying to do, which is custom build. Not take a generalized platform like CRM in every other industry and then try to spend two years plugging it in to get value out of it.
I’m not saying that’s not going to be required for the long run. It’s just that any large infrastructure investments are going to take two to four years just to get implemented, let alone the payoff period. Why not do something immediately that differentiates your health system from the consumer experience tangibly in a matter of months? That’s what we’re trying to offer and say, it’s really not about the technology. What is top of mind for those patients? We’re finding that it’s cost. It’s the worry of financial ruin. It’s a lack of transparency on any sort of quality metrics.
Patients ask us in our research for things like no surprise billing guarantee, satisfaction guarantee, transparent cash pay pricing, or things like best surgeons. I don’t know a health system that’s willing to show their own data on who’s the best surgeons, but I can tell you that patients would love it. Those are the types of things where we have to get out of a conservative mindset and start offering consumer-centric things that make us uncomfortable and take a bet that it is going to pay off. Because if we are really on the consumer’s side, they will pick us over any other system.
I don’t think that’s a crazy bet, because what would you want as a patient? If you or your parents need a CABG surgery and you have no information on any doctor about how good they are or their mortality rate, what’s it like? You’re just out there in the blue hoping that’s a good doctor over there. I hope they treat me nice. I wonder if I can get in the patient portal to track the progress? Doing little things to be on their side could be massive and saying, that’s really differentiated.
People want to self-schedule appointments with a provider who accepts their insurance, is conveniently located, has a good background, has time slots available, and accepts new patients. How well have health systems met that expectation?
It’s paramount. We gave a hype factor around AI, big data, and intelligence. I want to know, how many doctors do you have? Which ones are accepting new patients? What’s the earliest I can get an appointment? So few health systems in the country can answer this question.
Until you’ve done that, you haven’t earned the latitude to go build AI tools. If you couldn’t build a online scheduling platform correctly that is meaningfully used, if you aren’t doing 25% to 50% of your volume in online scheduling, what are you doing? What are you doing on the other stuff? Because that is such low-hanging fruit. It saves you money in contact center. It delights patients who don’t want to call for any of these things. It’s a massive opportunity to shift volume in the market share. There’s so many reasons to do it.
The only reason we don’t is that we’re not eating our own dog food. I don’t know many health system executives that are having to go through their own online portal and their own online scheduling, because as healthcare administrators, we all have access to calling the office to get us in, or we know Dr. So and So and we text them to get us in. We get to cheat. If we had to use our tools to try to book an appointment, nine out of 10 of us would be pulling our hair out because it’s so, so bad. You wouldn’t accept that from a barber. You wouldn’t accept that from a restaurant where you are reserving a table. Yet we say, “Sorry, but Dr. So and So doesn’t agree to open schedules. They think it’s unsafe or want to screen all patients first.” Well, too bad. Are we going to be consumer centric or not?
The fact that that’s all locked up in the EHR is a problem. We’re one of the only platforms that we’ve ever seen that can aggregate 50 to hundreds of providers and show you all their schedules sorted by next available. But it’s really all of that for that last step, sorted by next available, because we fundamentally believe that patients are going to pick their doctor based on who is available the earliest. Baylor has had that up on their website for three or four years. We’re starting to see one or two other health systems do it, but that basic capability is so far lacking and something that Amenities can do in a matter of weeks and months for health systems.
Just start there. That’s not an AI problem. Just get the logistics out and make all of primary care available for online scheduling. No questions asked, no exceptions. It’s the first thing we tell every health system. We’re going to make an amazing digital experience. Great, do you have online scheduling? No, not yet, but we’re talking to our docs about it. Our first question is, would you download the Pizza Hut app if you couldn’t order a pizza in it? No one’s going to use that thing you’re building, no one’s thinking about adoption and usage, and what will promote this and why is it differentiated?
We’ve started to talk to various health systems about memberships. One thing that we hear repeatedly is, we would like to do a virtual concierge program. That’s been done. That was done four years ago. You have to be better than One Medical, because One Medical is being advertised now inside of the Amazon app. Everyone has access to it for $9 a month. Are you going to be better than that and differentiated? Because if not, why even start? Would you use that? I feel like sometimes that we don’t want to ask this type of questions, and we need to, because that’s how we build something better.
What are the company’s goals over the next five years?
We would love to see a massive shift in the whole industry, ideally with us, Mission driven. We want to see the industry eliminate all of this friction. A lot of our products – provider scheduling, registration, and the digital front door – will help get the friction out of healthcare. Well within those five years, I hope we can start to demonstrate how market-making and how transformative memberships could be.
You’re seeing a ton of back and forth about too much MyChart message usage. “Well, I guess we have to to charge patients.” Let’s piss them off, because we’ve already pissed off the doctors. That is such an uncreative solution. Taking MyChart messaging away from patients is like now saying, “I’m sorry, it’s going to be 10 cents per text message” like when cell phones first came out. That’s literally where we are. The reality is that people want to use this.
This is a massive opportunity to create a new business model. I don’t know about you, but if I want to talk to my doctor exclusively, I would happily consider $9, $10, or $20 a month to say that I have unlimited messaging for them. They can actually create new services and capabilities. Now I would want more than that, but that’s the opportunity. That’s what I want to see us doing in the next five years, that we can point to a couple of core examples in the industry where they try something new and different, wrapped in a membership. We are seeing that mindset shift, where people are starting to say, that’s interesting. That could actually be transformative and move a ton of market share.Why don’t I try that first before my competitor does?
How do we massively change the dynamic? You have to go through health systems. Direct-to-consumer healthcare is nice, but health systems deliver the majority of care in this country. Two, you have to align incentives. We are not incentivized to compete on experience, but what if we were? Could that be a motivation to do a lot of new and different things?

























































'Samantha Brown points out that, “Healthcare, like every other industry, gets caught up in the idolatry of the ‘innovators.’”' I…