Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…
News 12/28/16
Top News
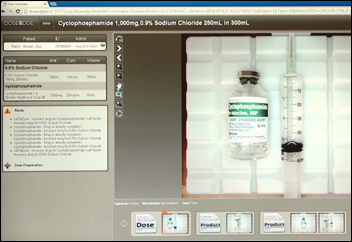
An Oregon district attorney says he was “on the verge of filing criminal charges” against St. Charles Medical Center-Bend (OR) for halting the use of Baxter’s DoseEdge barcode-driven IV checking system, thereby contributing to the death of an inpatient who received a mislabeled and ultimately fatal IV. The DA backed down when the hospital agreed to make safety changes.
The hospital said both McKesson and Baxter promised that Baxter’s DoseEdge system was compatible with its newly purchased McKesson Paragon EHR, but the hospital had to revert to manual medication checks when it found those claims to be untrue.
Hospital employees claim the hospital turned the DoseEdge system off in a cost-saving move and complain that the Paragon equivalent was too slow to be used.
The fatality occurred because of the usual “Swiss cheese effect” of having several safety steps break down sequentially:
- An expert pharmacy technician who had worked at the hospital for 37 years prepared the patient’s IV with the surgery muscle blocker rocuronium instead of the ordered seizure drug fosphenytoin.
- A pharmacist at the hospital didn’t notice the pharmacy technician’s mistake and approved the IV to be sent to the patient’s room.
- A nurse hung the bag even though it was clearly labeled with a “neuromuscular blocker” warning sticker that she says she didn’t understand.
- The patient was left unmonitored despite her physician’s order for continuous cardiac and pulse oximetry monitoring, which the nurse admitted she ignored.
- The nurse had to leave the patient’s bedside when a fire drill was called right after the IV was started.
The patient was found unresponsive 42 minutes later and was taken off life support two days after the incident.
The hospital has improved its processes, but it still won’t have a replacement IV checking system until it goes live on Epic in April 2018.
Reader Comments
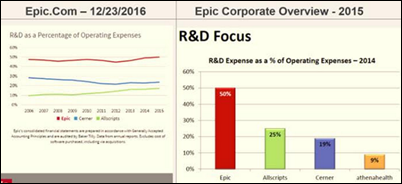
From Ex Epic: “Re: fun with numbers. Epic is replaying the hits related to R&D investment on their site, although they’ve at least left the Google and Apple nonsense out this time. Oddly, the site’s chart doesn’t match the corporate overviews shared across the campus. Epic’s 2014 and 2015 charts showed Allscripts spending more than Cerner, but their 2016 trend line (which includes those years) has Cerner outspending Allscripts. Which is it?” The trend line shows Cerner and Allscripts spending around 22 and 18 percent, respectively, in 2015, while the bar chart shows 19 and 25 percent. I wouldn’t put much faith in the numbers anyway since Epic compares itself with three publicly traded competitors that follow GAAP recognized accounting standards, while privately held Epic is under no such limitation. Companies can also elect to capitalize as R&D such items as allocated indirect costs (such as a portion of expensive office buildings), maintenance costs, support expense, and other gray areas that may provide little customer benefit. The bottom line (no pun intended) is how products perform and are viewed by customers regardless of how the vendor’s accountants book R&D expense, no different than with any other product. McDonald’s supposedly spends a gazillion dollars trying to invent new menu items that never catch on, but that R&D usually earns the company scorn rather than admiration and their food tastes the same regardless.

From Publius: “Re: Toby Cosgrove as a potential VA secretary. Since Cleveland Clinic is an Epic shop, does this increase the likelihood that the VA procures Epic as its commercial EMR solution, or is Cerner a foregone conclusion given the DoD project?” That’s a tough one. The VA and DoD have disdainfully declined to work together in advancing interoperability until mandated by Congress (and sometimes not even then), so while Cerner might make more sense, I would expect the VA to choose Epic just to be contrary. I think it’s a done deal that they will replace VistA with one or the other. Epic must still be stinging after losing to Cerner for the DoD’s MHS Genesis, so I assume they are using whatever DC influence they have (see: Paul Ryan) to bag the VA deal.
From Meltoots: “Re: integrating state prescription monitoring program (i.e., doctor-shopper) databases with EHRs. We asked our EHR vendor and the state of Ohio for this integration 14 months ago. Here is the click-type data entry nightmare we do today. Does anyone understand this?” Meltoots lists the required steps to perform the patient lookup in the PMP database, which might provide its own deterrent to opiate prescribing:
- Find the PMP’s webpage.
- Log in using the user name and password that constantly changes.
- Click OK that you understand this is private info.
- Click Search.
- Click and type in first name and last name (spelled perfectly), date of birth, ZIP code, etc., going back and forth locating the information in different EHR areas and then typing it into the PMP’s web form.
- Click and hope to find the patient.
- If the patient is listed, download the generated PDF file.
- Read the PDF and then print it to prove that you read it.
- Scan the PDF and attach it to the EHR chart to prove that you did it.
HIStalk Announcements and Requests
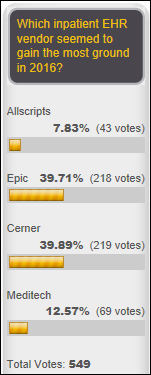
It’s a dead heat between Epic and Cerner in the admittedly subjective “who gained the most ground in 2016” category.
New poll to your right or here: is the increasing use of medical scribes good or bad? Polls need to be simple by design, so if you feel boxed in by my default answers, feel free to click the Comments link after voting to explain your position.

Fantastically generous donations from Epic Reader, Bucky Badger, Dr. J, Friend at Impact, and Bill – combined with matching money from my anonymous vendor executive and other sources – allowed me to fully fund these DonorsChoose teacher grant requests:
- 3D pens and printing supplies for Mrs. S’s elementary school class in Oakley, CA
- Makey Makey circuit kits for Mrs. C’s elementary school class in Walhalla, SC
- Two Chromebooks for Ms. V’s middle school class in Phoenix, AZ
- Two Chromebooks for Mr. B’s middle school class in Phoenix, AZ
- A Chromebook for Mr. S’s second grade class in Buena Park, CA
- 18 sets of headphones for Mrs. F’s kindergarten class in Hampton, VA
- Math centers for Ms. R’s kindergarten autism class in Newport News, VA
- Five Chromebooks for Mr. V’s high school biology class in Lake, MS
- Four science activity tubs for Mrs. B’s elementary school class in Fayetteville, NC
- A document camera, projector, laser printer, and other projection supplies for Mrs. A’s middle school class in Oakland, CA
- 3D printer pens for Mr. C’s robotics competition team in San Jose, CA
- Five Chromebooks and 15 sets of headphones for Ms. K’s fourth grade class in Detroit, MI
- Programmable robots for Mrs. O’s elementary school library maker space in Katy, TX
- A bamboo building block set for Mrs. B’s kindergarten class in Sumas, WA
- 30 sets of headphones for Mrs. D’s elementary school class in Sumter, SC
- $200 toward getting 10 Chromebooks for Mr. P’s 10th-grade class in Plant City, FL

Ms. L responded quickly even though Detroit schools were closed Tuesday: “I am beyond excited and grateful for your generous contribution! I can’t begin to explain how much these computers, headphones, and Flocabulary subscription will impact my students. We have been struggling with a lack of technological resources that has made it difficult to use the computer programs that are available to us in a meaningful and effective way. Your donation is helping bring up-to-date, WORKING, technology to our classroom. My students and I can’t say enough thank yous!”


Mrs. E from South Carolina says her students are learning from the programmable robots we provided in funding her DonorsChoose grant request. A snip of her email: “Many of the students come from low-income families that would never have had an opportunity to work with these tools if we didn’t have them at school. One of my students wrote in his thank you letter, ‘I have never in my whole life seen or touched a robot. They do really cool stuff.’ You have made a real difference in the lives of these students, not only by your donation in allowing the purchase of these materials, but also that someone cares enough about them to donate.”
Listening: new from 19-year-old Irish singer Catherine McGrath, who seems to be minimally known even though that should probably change. It’s sort of like pop-oriented US country music sung by Dolores O’Riordan of the Cranberries. Also: new from Columbus, OH-based science fiction-themed hard rockers Starset. One more: the amazing Christian hard rockers Skillet. Check out UK-born drummer-singer Jen Ledger, who plays with hair-flying, thrashing joy that reminds me of a female Keith Moon. Skillet’s tour starts January 28 and includes health IT towns like Madison, Philadelphia, and Indianapolis; they have over 1,000 Ticketmaster reviews with a five-star average and I’m pretty sure they would be entirely worth the $30 or so ticket price.
Last Week’s Most Interesting News
- The Department of Justice gives anti-trust clearance to the creation of a new health IT company by McKesson and Change Healthcare.
- CMS indicates that 171,000 Medicare-eligible providers will receive an EHR Incentive Program downward adjustment in 2017.
- HIMSS announces the retirement of President and CEO Steve Lieber, effective at the end of 2017.
- A JAMA-published observational study involving Medicare ICU patients finds that those overseen by female intensivists experience better outcomes than those with male doctors.
- HHS tweaks the Health Insurance Marketplace rules for 2018, with the most significant changes involving risk pools.
Webinars
January 18 (Wednesday) 1:00 ET. “Modernizing Quality Improvement Through Clinical Process Measurement.” Sponsored by LogicStream Health. Presenters: Peter Chang, MD, CMIO, Tampa General Hospital; Brita Hansen, MD, CHIO, Hennepin County Medical Center. The presenters will describe how they implemented successful quality governance programs, engaged with their health system stakeholders, and delivered actionable information to clinical leadership and front-line clinicians. Q&A will follow.
January 26 (Thursday) 1:00 ET. “Jump Start Your Care Coordination Program: 6 Strategies for Delivering Efficient, Effective Care.” Sponsored by Healthwise. Presenters: Jim Rogers, RN, RPSGT, director of healthcare solutions, Persistent Systems; Charlotte Brien, MBA, solutions consultant, Healthwise. This webinar will explain how to implement a patient-centered care coordination program that will increase quality as well as margins. It will provide real-world examples of how organizations used care coordination to decrease readmission rates, ED visits, and costs.
Acquisitions, Funding, Business, and Stock

A business site profiles the South Korea-based hospital-vendor partnership behind Bestcare 2.0, a hospital information system deployed in South Korea and Saudi Arabia that the group hopes to expand into the US market.
Decisions
- Marina Del Rey Hospital (CA) will switch from Cerner Soarian to Epic.
- Virginia Gay Hospital (IA) moved from CPSI to Epic In November 2016.
- St. Mary’s Hospital (CT) will replace McKesson Paragon with Epic in July 2017.
These provider-reported updates are provided by Definitive Healthcare, which offers powerful intelligence on hospitals, physicians, and healthcare providers.
Government and Politics
A New York Times opinion piece urges President-elect Trump to follow through on his previously expressed support for universal health insurance, warning him that Republicans in Congress (including his nominee for HHS secretary, Congressman Tom Price, MD) are giving him bad advice in pretending to support such a program while actually pushing “repeal and delay” without any plan of their own to replace the Affordable Care Act and thus driving insurers faced with poor risk pools out of the market. It recommends,
The crucial first step is to avoid repealing the insurance expansion without simultaneously replacing it. The new Congress comes to Washington next week, and its members should know where you stand from the beginning. It won’t work to promise millions of people health insurance on spec. If you avoid this trap, you can then push both parties toward a different version of universal health coverage.
FDA issues final guidance on post-market medical device cybersecurity.
Other

Lisa “Venture Valkyrie” Suennen posts her annual holiday song lyrics parody “Thriving Here in Venture Fundingland,” sung to the tune of “Walking in a Winter Wonderland.” She just took a job as managing director of GE Ventures.
A Black Book poll of C-suite provider executives predicts these trends for the first half of 2017:
- Hospital IT budgets will remain flat while physician practices will cut their technology spending an average of 13 percent from 2016.
- Electronic data warehouses will top the list of short-term priorities.
- Hospital interest in enterprise resource planning systems will be restored in a value-based care environment.
- Most hospitals haven’t budgeted for projects that would increase interoperability.
- Large hospital groups fear that cyberattacks will move upstream from the mostly small facilities that were impacted in 2016, expressing concerns about insufficient threat detection systems and the possibility of security alert fatigue.
- Hospitals are confident about their cloud application strategies even though most of them haven’t bought cloud-based disaster recovery solutions or don’t understand what they have purchased.
- Small-hospital CFOs will revise their RCM strategies and increase their focus on coding and clinical documentation improvement, with many of them considering outsourcing.
- Salaries for hard-to-find skills such as healthcare analytics, big data, security, mobile, and cloud technologies will jump as competition heats up and H-1B visa programs could be scaled back.
- Providers are interested in precision medicine, but nobody’s really buying systems to address it due to expected implementation difficulty.
The New York Times profiles the failed attempt of North Carolina physician group Cornerstone Health Care to transition to an ACO care model. The practice lost a third of its doctors (especially its high-revenue specialists) to higher-paying hospitals such as UNC Health Care; it had to borrow $20 million for capital projects such as new IT systems; and some of its doctors sued it in claiming that their compensation was reduced arbitrarily to cover debts incurred due to mismanagement. The practice ended up selling out to Wake Forest Baptist Health, which experts say is likely to raise costs as the focus changes from keeping patients healthy to feeding the hospital’s revenue-generating departments.
A CDC survey finds that physicians rarely collaborate with laboratory professionals in the 15 percent of encounters in which they aren’t sure how to order diagnostic tests and the 8 percent in which they received results they don’t understand. The primary barriers are that doctors don’t know who to contact or don’t have the time to do so. Physician respondents suggested adding lab ordering criteria to CPOE systems, publishing mobile clinical decision support apps, and adding lab professionals to multidisciplinary rounding teams.

Medical University of South Carolina will open an Apple-sanctioned retail computer store in its library that will offer discounted Apple and Dell products to students and faculty. It’s also considering using the store to provide health-focused technology, such as healthcare apps, to patients.
Sponsor Updates
- Horses for Sources and its research division cover a patient experience redesign project at Lawrence General Hospital led by Sutherland Global Services.
Blog Posts
- The New “21st Century Cures Act” Summarized (Impact Advisors)
- Patient Attribution and Care Teams – Managing Side-Effects of Population Health Initiatives (Optimum Healthcare IT)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.






I wouldn’t trust any numbers that Epic themselves gives. Judy has been known to “redefine” the truth
Agree with your assessment of the Epic R&D claims, but I think there’s one minor point to add. You’d expect Epic to account for their R&D spend in whatever manner they prefer, but that doesn’t solve for why Allscripts and Cerner’s numbers aren’t consistent. The logical answer is that they either made an error in their charting between 2015 and 2016 (unlikely), or they’re manipulating Allscripts/Cerner’s financial data. Why they’d change the financials (vs. just using what is on their annual filings) is beyond me, but it isn’t a good look.
The % differences are likely a difference between GAAP and Non-GAAP Operating Expenses. For example, stock based compensation would likely fall in the GAAP operating expenses where as the Non-GAAP would have them excluded. The real issue is that % spend doesn’t tell you how much or where those R&D $$$’s are concentrated. For example, Allscripts sold Touchworks to Optum. Much of their R&D spend may now be focused on that iPad enabled EHR. This really does you no good if you’re using Sunrise or Enterprise. Even with Epic is that 50% concentrated on their HIE or some other aspect of their product offering. Also, historically R&D spend does not correlate to innovation as IBM has out spend Apple in R&D spend for basically forever. Let’s keep focused on vendors like Epic that deliver good results and the good results will continue.
RE: R&D…Just another in the long line of salacious and unprovable claims. The bottom line on all of this vendor chatter is transparency, or a lack thereof. With Epic, you only know what they want you to know. With the field (athena, Cerner, Allscripts etc.) all are open to much more public scrutiny and review and even MEDITECH voluntarily reports some information to the SEC.
Cosgrove — By the time Cosgrove is confirmed and up and running the DoD will have multiple sites live. VA will have the benefit of evaluating the DoD project/Cerner on its merit… and can juxtapose that against what Epic accomplished with the Coast Guard. The GAO report being constructed on the failed Epic/USCG project should prove relevant as well. The historical agency politics will certainly matter, but there will be vendor performance to consider within the Federal sector before any RFP is issued.
Re: George W. – Here is Epic’s statement on what happened with the Coast Guard project (link below). Part of it reads “The Storage Area Network containing the software build was inexplicably corrupted once with no root cause, and was deleted once by Leidos staff – both times just before the system was ready to go live. We have never seen this occur in 35 years of installs. Epic rebuilt the SAN each time.” Very ironic that Leidos was partnered with Cerner on the DHMSM bid at the same time.
https://www.epic.com/epic/post/1778
Don’t forget that Leidos was brought in because the Epic project was failing and behind in the first place. And I’m not sure Epic blaming another firm via their own blog is the best way to account for the facts…Do you really believe that Leidos sabotaged the project, or are you just insinuating for effect?
No, Leidos was not brought in later. They were part of the original bid.
No more “Lying George W.”, thought you’re lies were done with long ago.
There is foul play here. Leidos is just lucky Epic didn’t press it at the time, but with an actual OIG investigation, Epic might decide to just go for it and see where the cards fall.
They likely didn’t press it at the time because the DoD was still an open procurement.
Now might be the perfect time to demand accountability for a Vendor (Epic) whose CPARs were “Excellent” in almost all regards through the project had the rug pulled out from under them at the last minute in the closing hours of a procurement that hugely benefited Leidos.
Mr. H
UCLA opened a full Apple Store back in the late 90s. I bought my first MAC there. They have been providing MAC and Microsoft student discounts since then as well. They were also one of the first universities to completely outfit the main college library with next-gen Apple products. Too bad their Epic install is a piece of $hit.
Uhh USC is only 18 years late. Yes I know it’s Uni of South Carolina, not USC aka Southern Cal, but I’ll jump on any deragatory reference I can make about the U$C Toejams uh I mean Trojans.
Liar Liar Pants on Fire,
Per the Politico article last May the CG bid the contract direct to Epic as prime in 2010. And didn’t bring in additional support until 2012 – which included Leidos, InterSystems, Lockheed and Apprio. Maybe I’m wrong, but seems Leidos wasn’t part of the original bid team and at a minimum they certainly weren’t the prime. I pasted in portions of the article that are relevant.
In September 2010, the Coast Guard bid out the contract to Epic Systems, then added an array of other contracts to software vendors and consultants to help implement it. Since 2010, the agency spent, on net, just more than $34 million on health IT.
Cullen also found it odd that the Coast Guard didn’t hire consultants to implement the new system until September 2012. The service ended up hiring Leidos, which also maintained its old EHR.
Government contracting is hard. Epic may or may not figure it out. Odds are that won’t really matter. Might be better for Epic if Cerner is distracted by fat government contracts.