Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…
Monday Morning Update 8/19/13
From DanburyWhaler: “Re: Norwalk Hospital. No longer hooking up with Western Connecticut Health Network, now part of Yale-New Haven. Stay tuned for lots more consolidation in Connecticut” That would be interesting since Norwalk just signed up as a WCHN affiliate in January.
From Jon: “Re: HIMSS. They emailed members about the ICD-10 Playbook, and when I click the links, I get the infamous registration form before I can view it. It is sponsored by vendors, which is appropriate, but it should be available to all members with no strings attached for all the money we spend on dues. Now we will be bombarded with sales calls. No, thanks. I think my HIMSS membership days are over. Hopefully others will join me in sending a message.” HIMSS has gotten so commercial and so intertwined with its vendor members that I treat them like any other vendor, i.e. I always assume anything they send is spam. I’m rarely wrong on that. All the resources that require registration are on the site of MedTech Media (Healthcare IT News, Government Health IT, etc.), a private company of which HIMSS bought the majority position of shares in 2011.
The more important debate to me is this: are vendors doing themselves a favor by hiding their promotional material behind a registration form? Vendors think this way: we need leads, and any names we can get, even of people with marginal interest, make us feel more successful. I think this way: why in the world would you make it harder to see your advertisement? Nobody wants to be cold-called just because they took a quick look at a white paper. I would bet people often do as I do in just inserting phony contact information to avoid the dreaded phone call (note to vendors: if you are trying to reach a CIO named Scatman Crothers who used a phony email address, that’s me.) Don’t listen to your marketing and sales people – put your stuff out there where everybody can see it. Do the right thing and the HIMSS problem goes away with it.
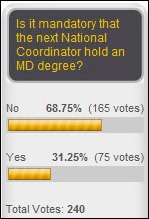
Two-thirds of respondents say it’s OK if Farzad Mostashari’s replacement isn’t a physician, although most of the respondents probably aren’t members of Congress who may expect to see an MD in charge. New poll to your right: will the FDASIA report help improve patient safety with healthcare IT? Vote first, then click the Comments link at the bottom of the poll to explain your thoughts because “yes” or “no” votes don’t create rich debate.
Speaking of FDASIA, I made that the lead item in “This Week in HIT,” a partly serious, partly snarky weekly news update that I’ll do on Fridays. It will focus on the most important stories of the week, which admittedly aren’t all that fascinating at the moment given the summer doldrums before the inevitable September pickup (hint to vendors: it’s a great time to make announcements.) Long-time readers will remember the format from the Brev+IT weekly newsletter I used to send out until the volume of work overwhelmed me, much of which went toward coming up with Onion-like headlines. People have asked for a weekly summary of just the major news items, so this is it.
Thanks to the following sponsors, new and renewing, that recently supported HIStalk, HIStalk Practice, and HIStalk Connect. Click a logo for more information
Wake Forest Baptist Urgent Care – Clemmons goes live with UrgentQ, a “fastpass for healthcare” that lets patients choose an open visit time and receive text message updates of when to come in. It’s from Lightshed Healthcare Technologies, a new company founded by Dialog Medical Founder Mike Burke.
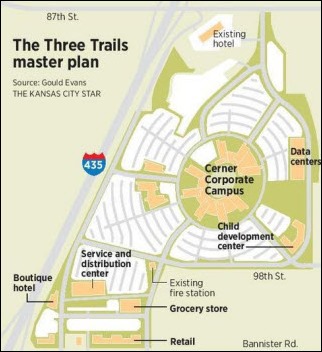
Cerner will develop the biggest office project in Kansas City history if its plans for the former Bannister Mall are approved. The campus will cover 4.5 million square feet on 251 acres and will be valued at $4.1 billion upon completion. It will house up to 15,000 employees. Cerner wants $1.2 billion in tax incentives to build it, offering to chip in $2.9 billion of its own money.


Readers have asked for an update on the HIPAA Omnibus Rule, for which enforcement begins in just a few weeks. I publicly solicited pro bono volunteers to to review the changes via Webinar. Doing so will be a couple of excellent presenters from The Advisory Board Company: Associate General Counsel / Privacy Officer Rebecca C. Fayed and Information Security Officer Eric Banks. Sign up for The HIPAA Omnibus Rule: What You Should Know and Do as Enforcement Begins, which will be held on September 10, 2013, from 2:00 to 2:45 p.m. Eastern. I reviewed their slides and they are excellent in the usual Advisory Board fashion – very meaty and to the point as they cover changes related to business associates, breach thresholds, and everything else covered entities need to know and do. This is a non-commercial presentation offered strictly to benefit readers by Rebecca and Eric. I appreciate their involvement.
The West Virginia Health Information Network has added several hospitals recently, bringing its total to nine.
Louis Kraml, CEO of Bingham Memorial Hospital (ID) pleads guilty to stalking charges for illegally wiretapping a former hospital physician, aided by three of the hospital’s IT department employees. Charges were dropped against two of the employees because they were following the instructions of IT Director Jack York, who had been accused last year of running a bogus consulting company that was charging the hospital for IT services. The court has issued a warrant for the arrest of York, who didn’t show up in court. The charges aren’t mention on LouisKraml.com, the CEO’s official website.
HIMSS urges HHS to start Meaningful Use Stage 2 as scheduled, but suggests extending the attestation window to 18 months.
The Fort Lauderdale, FL newspaper covers the use by several hospitals, most of them VA facilities, of the GetWellNetwork patient engagement solution.
The National Science Foundation issues a five-year, $10 million cybersecurity grant to Trustworthy Health and Wellness program that will develop tools for authentication and privacy, malware detection, and medical IT auditing. Experts from Dartmouth, Johns Hopkins, University of Illinois at Urbana-Champaign, and University of Michigan are on the team.
Sidney Health Center (MT), a 25-bed critical access hospital, will implement Epic as part of an agreement with Sanford Health (ND).
Vince commences his HIS-tory coverage of Cerner, aided by Neal Patterson (who responded quickly and warmly to Vince’s inquiry) and the archives of Cerner’s April Martin. The details they provided are fascinating.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.






















So Cerner wants the state/local gov’t to cover nearly 30% of the development costs? I would love to see some aggregrate numbers around it but it seems like this is becoming more and more of a problem and larger employers are becoming ever more bold/greedy on the amount they are seeking from local/state gov’ts in order to ‘create jobs.’
What Cerner is doing is not greedy – it’s smart – if you were from Kc you would know the area they want to develop is terrible. It was the site of a mall and shopping area that had to be torn down – the mall had towers were guards would sit to watch for theft….not a great area… It’s would be amazing to see that area developed and alive again.
The state of Mo and the city would be wise to work with Cerner – or we (Missouri) will lose a major employer to Kansas….
The Southeast side of our city died long ago and this would increase property value, create jobs, and be a real opportunity – if you were from KC you would understand.
And no….. I don’t work for Cerner….but I do want the state to work with them.
I don’t mind that local governments use tax financing to support business, but I do mind that they neglect to remember that it happened and then whine and moan and complain about the cost of doing business.
The taxpayers have already filled Cerner’s coffers via the government largesse aka HITECH. The double whammy on the taxpayers is despicable. Hopefully, the Mo government officials will read your blog and the MAUDE database over at the FDA on Cerner.
Cerner taking more money from taxpayers to produce unusable software? Shocking!
“Forbes ranks Cerner #13 on its list of the world’s 100 most innovative companies, as measured by the difference between its market capitalization and the net present value of cash flows from its existing businesses.”
Innovative or overpriced?