Yeah i'm not sure this ruling really moves the needle on Epic's behavior at all, the non-competes were always believed…
Monday Morning Update 1/30/12
From You Know Who: “Re: RelayHealth. Jim Bodenbender out, announced abruptly on phone call. Jeff Felton, who ran the RelayHealth Pharmacy group and was a transplant from McKesson San Francisco, is taking over the entire division.” That appears to be true from the company’s management team page, on which Jeff Felton (above) is now listed as president.
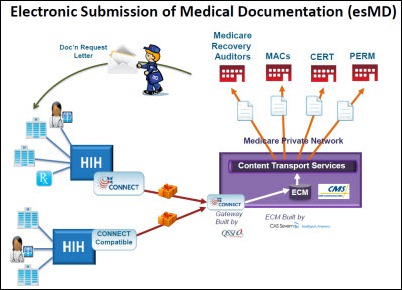
From RAC Frustration: “Re: electronic RAC responses. I see that Medical Electronic Attachment (MEA) has become the latest company to be certified by CMS. I am curious how many HIStalk readers will use the esMD (electronic submission of medical documentation) for RAC and MAC responses?” MEA’s progam uses an NHIN gateway to send electronic responses to CMS’s post-payment audit requests of several flavors (RAC, MAC, CERT, PERM, and ZPIC.) I’m interested in how much transaction volume the average hospital will experience to keep CMS happy once esMD Phase 2 goes live in October and all documentation requests will be sent electronically. Comments welcome.
Surely the calendar is playing a cruel joke: it can’t be just three weeks until the HIMSS conference, can it?
My Time Capsule editorial this week from five years ago: Want Physicians to Use Systems? Standardize Screens Like You Do Back-End Databases. A free sample: “Hospitals never seem to get how illogical it is to physicians that every hospital buys a different system, but expects community-based doctors who cruise in for an hour a day to master all of them without burning up more hours of their self-employed day. They seem puzzled when doctors jeer at their zealous requests to bone up on Cerner when he or she is fuming at Eclipsys across town and McKesson at the university hospital.”
Listening: reader-recommend James, which I would characterize as jangly Britpop with strong vocals. They (it’s a band, not a guy) remind me of the Smiths. They aren’t totally obscure, having sold 25 million albums in their 30 years. They probably would sell more if they had a more search engine friendly name, although come to think of it, that’s another similarity between them and the Smiths.
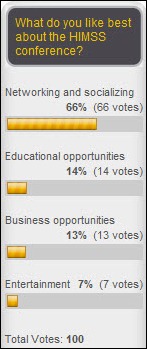
A lot of money and effort is spent putting on the exhibit and educational tracks of HIMSS, but that’s just to provide the backdrop for the real reason people attend: to connect with folks for business and pleasure, two-thirds of respondents said. New poll to your right, as suggested by a reader: what reaction do you have when you hear that a vendor uses offshore programming resources?
Thanks to CSI Healthcare IT, supporting HIStalk as a Platinum Sponsor. The company is a leading national provider of IT and training professionals, both contract and permanent. The company’s team of 75 recruiters can often find local qualified resources, minimizing billable travel expenses to the client. Its pricing model has saved health system customers such as Sutter, Baylor, Texas Health, Clarian, and Sentara up to 60%. The company is vendor neutral, providing resources for projects involving McKesson, GE Healthcare, Allscripts, Epic, Cerner, Meditech, NextGen, and others. It can handle work ranging from providing a single resource to managing the projects of large health systems, also offering a specific package called Epic Community Connect that helps health systems provide Epic’s ambulatory systems to community practices (marketing, contracting, readiness assessments, implementation, and support.) Thanks to CSI Healthcare IT for supporting HIStalk.

Federal CTO Aneesh Chopra resigns and is expected to run for lieutenant governor of Virginia. You aren’t surprised if you read HIStalk on January 13, when my non-anonymous, well-placed informant chose the fantastic phony name of DeepThrowIT to tell us that Chopra was heading out. I think that might have been my first non-healthcare IT big scoop rumor.
I recently quoted some Epic facts provided by Chief Administration Officer Steve Dickmann in a recent talk he gave to a Madison group. The full video is here, from which I pulled a few more:
- The company started in a basement in 1979 doing UW psych department work.
- Epic went from 2.5 employees in 1979 to 30-40 employees in 1994, but then changed direction to focus on the electronic medical record.
- The product was changed from text-based to a graphical GUI in 1994, the same year when the database was scaled up for large enterprises.
- Epic Web came out in 1997; MyChart in 2000.
- The company gained competitive advantage from Y2K because it had minimal remediation to accomplish while its competitors had to redirect resources to work on that problem.
- Epic also gained competitive advantage from being in Wisconsin, which was an early adopter of large integrated delivery systems.
- Epic does not subcontract or acquire software; everything was developed in Wisconsin.
- The original motto was “Do good, have fun.” The “make money” part was added later.
- Epic focuses on large hospitals and clinics, children’s hospitals, and academic hospitals and turns away other prospects. The only exception they will make is for hospitals located in Wisconsin.
- Epic doesn’t do acquisitions because they would have to rewrite the code anyway to keep a truly integrated product.
- Competitors have 20-30% of their employees doing sales and marketing, while Epic has 1%.
- Epic’s culinary team has 70 employees and it also staffs its own horticultural team. It does not contract those functions out.
- All of Epic’s implementers fly out Monday afternoon, which ties up a good bit of the Madison airport’s capacity with 600-700 people all leaving at about the same time.
- Each customer has an assigned tech support team that knows the customer’s people and systems. The team is available 24×7.
- 91% of the HIMSS EMRAM Stage 7 hospitals use Epic.
Supporting HIStalk as a Platinum Sponsor is Versus, which offers real-time location systems for patients, staff, and equipment. Hospitals use that information to automate workflow, improve efficiency, increase patient safety, boost patient satisfaction, and increase revenue. The company provides interesting examples: (a) advancing patients to the next level of care based on events, such as completed labs or EKGs; (b) locating telemetry patients in distress wherever they are; (c) alerting the physician when patients are ready to be seen; (d) reminding staff to wash hands; and (e) alerting housekeeping to clean the room when the patient’s badge is dropped into the discharge bin. The Traverse City, MI company has been around for over 20 years, with its combined infrared/radio frequency system being endorsed by the American Hospital Association. Hospital customers have documented improvements such as cutting equipment losses from $1.5 million to $40,000 year, eliminating the need for clinic waiting rooms, reducing telephone calls by 75%, and increasing bed capacity by 25% with no construction. Interesting stats: the company has over 600 facilities using 500,000 of its components to track more than 1 million patients per year. The big announcement a few weeks back was that The Johns Hopkins Hospital chose Versus to manage staff and assets in real time for some locations after a three-year pilot of several RTLS systems, with additional deployments scheduled. Thanks to Versus for supporting HIStalk.
The Peace Corps has an RFI out for an EMR product, just in case you’d like to sell them one. They’re actually looking to have OpenEMR customized, along with Microsoft Dynamics 2011 and BizTalk for reporting.
In England, Homerton University Hospital allows its original NPfIT contract for Cerner and BT expire and signs its own seven-year extension directly with Cerner, declining to open the opportunity to other vendors because of its working relationship with the company.
The Bipartisan Policy Center releases its recommendations for using healthcare IT to improve care and reduce costs. Quite a few industry names served on the task force and provided their input. Some of its observations and recommendations:
- Even with new delivery models, the healthcare system continues to financially reward procedure and patient volume rather than better care. Recommendations: purchasers and plans should reward care that is higher quality and lower cost, incorporate those models into Medicare physician payments, expand pilots of new care models, and share lessons learned with private sector pilot projects.
- Despite a lot of HIE activity, not much patient information is actually being exchanged. Recommendations: improve the HIE business case by adding more stringent information exchange requirements to Stage 2/3 of Meaningful Use, develop long-term standards that make sense for healthcare delivery, assess the level of information exchange that is occurring, do more work related to two-way data exchange, and clarify the role of health information exchange in the several programs funded by HITECH.
- Consumer engagement with electronic tools is minimal. Recommendations: raise public awareness, help providers engage their patients to use technology, improve the usability of consumer tools and provide easy data import/export for consumer-facing applications, launch an awards program for consumer tools outcomes, share lessons learned, ramp up Meaningful Use requirements to include more consumer tools, and offer incentives to chronic disease patients to use electronic tools to manage their health.
- EHR and Meaningful use adoption is still low. Recommendations: raise awareness of incentive programs and expand RECs and similar programs, clarify Meaningful Use requirements, roll out lessons learned form federal programs to the whole industry and not just government contractors, encourage sharing of best practices, and improve EHR usability.
- Consumers are worried about privacy and security. Recommendations: require all entities that use PHI to comply with policies at least as stringent as HIPAA, clarify government guidance across agencies, development a national strategy for patient identification (a national ID was not specifically mentioned), and issue common sense security practices to providers.
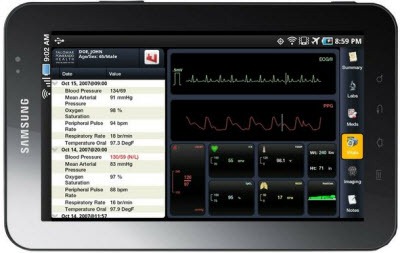
I’ve previously mentioned the MIAA EHR mobile viewer app developed by a three-person Palomar Pomerado Health development team for its own use with its Cerner systems. A preview at a Toronto mobile healthcare conference generates interest, with the app going to pilot in March. The hospital hopes to commercialize it. Said a Canadian hospital IT director at the conference, “We need to look seriously at how a publicly-funded hospital in the States has been able to advance their technology like this when we seem to stumble on things like policy and rules.”
The Pennsylvania Health Department finds that nurses at St. Luke’s Hospital overdosed three patients in the past two years by incorrectly programming their PCA pumps. Hospital employees said the hospital did not require training on the devices.
An article covering successful businesses that did not use outside financing provides an example in eClinicalWorks CEO and co-founder Girish Kumar Navani, quoting him:
I don’t foresee leaving the company for at least 10 years. I would like to leave it a private company with no external investors and absolutely no thoughts whatsoever about Wall Street. I am having fun and take great pride in my freedom. There is no reason I would give that up. We are a cash flow positive company. We have recurring revenues and no debt. We have a large customer base that is growing exponentially.

Compuware says it will take its Covisint subsidiary public in its next fiscal year, which starts in April. Covisint, which has $74 million in annual revenue, offers an exchange platform that connects hospitals and practices, including services for identity management, collaboration, master patient index, and record location.
Vince’s latest HIS-tory: Part 2 of Health Micro Data Systems.
A column in The Atlantic revisits a 1995 article it published about Newt Gingrich, saying that some of his goofy, overly dramatic “we are at a crossroads” ideas (like colonizing the moon) prove that he can’t separate something that sounds cool if given little thought from pushing the government into spending huge amounts of money just to find out how cool it is or isn’t, even though the free market is better equipped to make that call. Healthcare technology was mentioned in that 1995 article:
Gingrich also thinks health care technology is cool. Serious students of this subject worry that insurance insulates patients from the cost of technology, thus yielding lots of high-cost, low-benefit use and in turn steering too much of society’s resources to the further development of such machinery. But Gingrich wants more. In 1984 he wanted more cat-scan machines, and he wanted the government to provide a $100 million incentive for the development of user-friendly dialysis machines–even though "there are already companies and researchers interested in this problem." The point here isn’t that Gingrich will now waste tons on technology. The current political climate will restrain this tendency. The point is that–in case you hadn’t noticed–there is little careful thought underpinning his enthusiasms, nothing solid beneath his unshakable self-assurance and his intense disdain for disagreement.
More news: HIStalk Practice, HIStalk Mobile.







Vince lost me and many others when he first wrote “…while climbing Mt. Everest ….”
Now it’s politics.
There goes the sheeps clothing.
Re: Epic Facts.
Having work on the provider side with Epic’s technical services team, I can guarantee you that I could not always reach my Tech person 24×7 … she had 4 other accounts.
Re: Epic Facts. Cadence, their scheduling module, was originally written by contractors, not employees and not in Wisconsin.
I think Jeff Felton’s title already was President – over Pharmacy, something he earned from his transfer from leading Zee Medical I’m sure. Sad to see Jim go, but this is probably the best thing for RH. The highly fragmented mini-business unit structure at RH and McK leads to inefficiency, duplication, arrogant leaders and competing business strategies within the same company. RH might be more of a competitive threat if they could have the horses pull in the same direction for once.
Happy to be on-board! Thanks for all the great work you do!
Love Mr. HIStalk (and thanks to the Mrs. for sharing you), Inga, Mr. Marx, Dr. Jayne, WNA–everything! First stop of the day for many of us at Versus!
With integrity and honesty in marketing being critical as we come up on HIMSS, Peter’s (above) comment on Steve Dickmann’s speech is intersting. It seems to say that Steve was not being honest about a key value of his firm.
Peter, could you please provide more detail on your comment that “Cadence, their scheduling module, was originally written by contractors, not employees and not in Wisconsin.”
“Epic focuses on large hospitals and clinics, children’s hospitals, and academic hospitals and turns away other prospects. The only exception they will make is for hospitals located in Wisconsin.”
This would appear to be inaccurate, since Epic implementations are well-documented in smaller/mid-size community hospitals outside of Wisconsin that are not part of IDNs. Epic doesn’t walk away from anybody, regardless of what they say, at least not nowadays. Not that it really matters, but let’s be honest about the myth of selectivity. It’s not an honor if Epic allows you to buy their software – it’s marketing.
I agree with David and Peter. We need some spandex transparency.
Re: From RAC Frustration: “Re: electronic RAC responses…. Comments welcome”
As a consultant, I cannot provide information regarding the average hospital’s transaction volume. However, I can attest to an enormous amount of paper going to the various audit review contractors.
Currently (Phase I), review contractors request medical documentation by sending a paper letter to the provider. Providers submitting the requested records can 1) mail paper; 2) fax, which usually starts and / or ends in paper; and, 3) electronically send medical documentation, again, which usually starts and / or ends in paper. This is true in provider organizations with complete EHRs because few product systems have the necessary “release of information” or “claims submission” capabilities that allow all or some of the required documentation to be transmitted electronically with the push of a button.
Consequently, 3rd party, Health Information Handler companies (the MEAs, HealthPorts, NaviNets, etc.) are required to make this happen, especially when the claims will be selected for review in Phase II. The HIPAA 5010 X12 837 Claims Transaction (Dental, Professional, Institutional) should have an impact.
Peter-do you have any details to back that up, or at least a source? I was under the impression that Judy wrote most of the original code for Cadence.
Cadence just LOOKS like it was written in house. That bad 90s windows app look….. like a MUMPS programer self learnt VB… No. It’s better than that. Just. Document flowsheet builder was written by an old M developer though. Must have been. Can anybody confirm?
Re: Cadence
Completely wrong. Cadence was developed in-house – I was there. Judy did not write the code, though she wrote a lot of the original chronicles code.
Cadence has tended to be the bad boy application in the past, although that is starting to get reined in. Just because it was developed in house doesn;t mean that it wasn’t siloed enough to cause issues.