The ruling does seem to actually touch on things like UserWeb access "...the final rule applies to terms and conditions…
Readers Write 8/31/10
Submit your article of up to 500 words in length, subject to editing for clarity and brevity (please note: I run only original articles that have not appeared on any Web site or in any publication and I can’t use anything that looks like a commercial pitch). I’ll use a phony name for you unless you tell me otherwise. Thanks for sharing!
Meaningful Use: Specialists Still Not a Priority
By Evan Steele
The HIT Policy Committee’s creation of a new Quality Measures Workgroup last week is the most recent in a string of actions confirming that meaningful use has not been defined meaningfully for specialists — and that it is not likely to be. Despite the fact that this new workgroup is charged with prioritizing Stage 2 quality measures and analyzing gaps in Stage 1 criteria, the 18 physicians selected for the 24-member group are primary care providers* — a fact that surely raises concerns among specialists.
The appointment of this workgroup comes on the heels of a growing response to the Stage 1 definition of Meaningful Use from specialists and their professional organizations, commenting on the lack of fit with the way specialists routinely practice. Every one of the six core clinical quality measures are primary care-related, and many specialists will be hard-pressed to identify three of the 38 additional clinical quality measures that are relevant to their practices.
At last month’s HIT Policy Committee meeting, committee member Gayle Harrell commented that much of the input gathered from the specialist panels convened last October seems to have been ignored, She contended that in the final rule, CMS made it more — rather than less — difficult for many specialists to comply with Meaningful Use.
This position was echoed by Thomas C. Barber MD, EMR project team leader of the American Academy of Orthopaedic Surgeons (AAOS) in discussing the Academy’s EMR position statement in the most recent issue of AAOS Now:
Orthopaedic surgeons will have great difficulty in meeting the current 25 Meaningful Use standards. Orthopaedics would derive greater benefits from standards promulgated by our medical specialty society rather than a set of generic requirements that mostly do not apply to musculoskeletal patient care.
This is not a new issue. The primary care focus of the legislation and regulations has been intentional from the outset. President Obama appointed an internist, David Blumenthal MD, to spearhead the program. There was only one private-practicing specialist among the committee members that crafted the recommendations to CMS.
It is not surprising that the Meaningful Use criteria do not reflect the practice patterns of specialists. Federal funding to assist physicians with EMR adoption has been directed towards primary care. The $357 million allocated for Regional Extension Centers, for example, was earmarked to “provide outreach and support services to at least 100,000 primary care providers and hospitals.”
The definition of Meaningful Use is not the only obstacle for specialists. The EMR products themselves are not tailored to the needs of specialists. The AAOS EMR Position Statement correctly suggests that in developing certification standards, it is essential that “the different needs and uses of EHR by disparate medical specialties should be recognized. In particular, the differences between surgical specialties and primary care specialties should be acknowledged.“
Unfortunately, because the certification criteria are linked to the Meaningful Use requirements, they are similarly primary care-driven. The EMRs most likely to be certified for Meaningful Use are predominantly those that were created and developed for primary care physicians — those of vendors that, from 2004 until recently, have devoted their development resources to meeting CCHIT’s 467 largely primary care-focused criteria. The AAOS statement continues: “Many systems are geared toward primary care medical practice, which can limit the utility of EHRs for specialty surgical practice.”
Specialists are no different from other physicians in their desire to participate actively in the evolution of the country’s medical care delivery system. But until Meaningful Use is defined in a way that is applicable to the way they deliver that care, they will participate on their own terms — adopting specialist-focused EMR technology that increases their productivity and enables them to provide the highest quality care and service to their patients.
* Includes internists, family practitioners, pediatricians, preventive medicine, an internist/hematologist, and a psychiatrist.
Evan Steele is CEO of SRSsoft of Montvale, NJ.
Safeguarding EMRs Against System Failure or Downtime
By Arthur Young
Using time-saving information technology and automated patient records management ensures clinicians have faster access to the most up-to-date patient information, enabling timely diagnoses and treatment and maintaining a high quality of care. However, if the network goes down, the system fails, or a planned or unplanned system downtime occurs, clinicians are unable to access critical patient information.
Whether they are planned or unplanned, system downtimes can occur for any length of time — from a few minutes to a few days. Downtimes can also be very costly if there is no system for preserving and accessing up-to-date patient information and maintaining uninterrupted patient care. Healthcare organizations have implemented systems for recovering from disasters, but not for protecting data and continuing operations during downtime. Without such a system, downtime can become more than an annoyance — it can be a life-threatening event.
Distinct from disaster recovery — which helps get systems back up when they go down due to a power outage or property damage — business continuance keeps vital business operations running at or near normal capacities in the event of any network or system downtime. That includes the downtime that occurs while disaster recovery mechanisms are being executed.
There are various solutions available that can help healthcare organizations remain functional during downtimes. However, they have drawbacks. Redundant or fault-tolerant systems can keep computers running and available during a system failure or power outage, but if they are the only system being used for business continuance and the network also goes down, clinicians will not be able to access patient data. Printing patient reports periodically allows clinicians to have the current data on hand, however it is a time-consuming and cumbersome task that diminishes data security, not to mention a waste of paper, ink, and other resources.
To maintain access to patient information from the location its needed, healthcare organizations need to select a business continuance approach that will provide the most protection in the most circumstances. Ideally, a business continuance solution should enable healthcare organizations to do the following:
- Identify critical information and automatically distribute it to areas it will be needed in the event the HCIS is unreachable;
- Ensure the information is secured but available on local machines;
- Maintain seamless operation in the background, notifying administrators of any interruptions; and
- Eliminate the storage of data in paper form, saving paper, ink, and printers.
Intelligent report generation and distribution decentralizes data in the event of downtime by sending the latest reports from the HCIS to its system and creating secure databases in multiple locations. The information is indexed in the database so clinicians can search and find the data they need whenever they need it.
With access to critical data during periods of system failure or extended downtime, clinicians can provide uninterrupted care and healthcare organizations mitigate risks to patient safety. Patients can be assured their health records are up-to-date and secure and confident they are receiving the best possible care.
Arthur Young is the president of Interbit Data of Natick, MA.
Ode to the Dumbwaiter and Robo-Butt
By Frustrated Farmacist (Female)
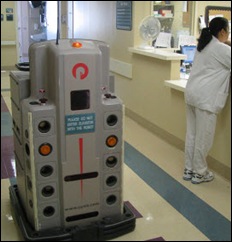
I saw your blurb about the Aethon TUG delivery robots installed at El Camino Hospital. The old ECH had an awesome dumbwaiter delivery system in place.
It is rumored that the Aethon TUG delivery robot solution was something of an afterthought that came six agonizing months after the grand opening of the $470 million hospital. Apparently earlier plans to integrate a delivery system may have been (ahem) overlooked. You can see from ECH documents that the robot contract was drafted in January 2010, several months after the new hospital opened. Early reports said the robots didn’t work for all departments and some ended up using volunteers, auxiliary staff, temporary workers, and other solutions to get medications and lab materials delivered.
$470 million and NOBODY initially planned an integrated medication delivery and lab transport system for a brand new, ultimate-in-high-tech 400-bed hospital! It doesn’t take too much imagination to extrapolate how important timely medication delivery is in the patient care scheme of things and why it’s the top complaint and employee satisfaction issue for nurses.
ECH’s competitor down the road has been using a similar robot system from Pyxis for the PAST 22 YEARS. It’s on its third generation, fondly named Robo-Butt. He travels in elevators and down halls to six floors and 15 departments. He is guided by sensors in the walls and speaks aloud to nurses to alert them when he arrives and when he commandeers the elevator. He steers around obstacles. His compartments are locked and secure, requiring a numbered password to open. He’s powered by six car batteries that are recharged and swapped for backups 2-3 times daily.
He breaks down every now and then. The elevators break down more often, grounding him on the first floor. Pyxis no longer supports these robots, so parts were scrounged from the basements of other hospitals and from a hospital supply house in Hawaii. But Robo-Butt WORKS. Here’s a picture of this bad boy:
The average hospital pharmacy department dispenses at least 40% more meds than were ordered because of late deliveries or items that are misplaced. The overhead and amount of wasted labor and supplies is unacceptable and frustrating for everyone involved, including the patient, nurse, doctor, pharmacy, and departments like lab and surgery that are held up because of medication delays.
With pneumatic tubes, you place meds in padded bullets and shoot them to the receiving department. Fragile ampules and vials can be broken — think about Epogen, a blood booster whose fragile proteins are destroyed by a violent trip in the tube system. It used to cost $6,000/vial and is still in the $600-900 range. Can I tell you how many bullets have exploded inside the pneumatic tube tunnels? Can I tell you what I think about the ER department tubing patient urine and blood samples to the lab inside this system?
We still have bullets that wind up in the basement due to malfunctioning suction or drivers. It’s hilarious when it’s a $45,000 rattlesnake venom antidote. But the bad part is that sometimes meds lie in piled up bullets in the tube receiving bin. Worse, the staff goes to send an “empty” tube to lab or ER and accidentally send a bullet filled with meds. The worst part is there is no “track-ability” or accountability — we can never tell whether someone received a bullet. If they “say” it never arrived, we have to send it again.
Here’s why I think dumbwaiters may be the ultimate smart medication delivery system with the fastest turnaround times, the least amount of waste, and minimal lost meds and lost charges. The pharmacy staff places labeled / bagged medications into little sectioned trays (like your silverware drawer’s insert) and leave them in the little locked elevator. The nurse that needs meds comes to her department’s locked elevator door, calls up the tray, and REMOVES ONLY HER PATIENT’S MEDS. She leaves the other meds in their little slots.
Think about this. You don’t have one nurse removing meds for her entire department and then misplacing them, storing them improperly (oops, that expensive IVIG that cost $20,000 belonged in the refrigerator?) or just putting them in her POCKET and forgetting to put them in the med room altogether. Then the Pharmacy can call the dumbwaiter down later and retrieve unused meds, credit them back, and recycle them.
You can imagine that the number of missing med phone calls drops in half. Anyone in the pharmacy can check the dumbwaiter and see if missing meds are there before re-making them. Can I tell you how much time I waste every day re-doing the same missing med that simply gets misplaced or misdelivered and there’s no way to track it? It’s cheaper to bag up another blood pressure pill with the patient’s name and send it again sometimes. And then we get to retrieve all the duplicates, sort them, and restock them in the pharmacy bins…
I have nightmares about this.
A reliable well-planned medication delivery system is worth $$$ millions and makes up 80% of the nursing / customer satisfaction basis. I swear this is true! Any healthcare organization that builds a state-of-the-art facility without planning a delivery system is completely ignorant.
Done with my rant. 😉




While I agree with Evan Steele about CMS ignoring the particular needs of most specialists when it comes to handing out ARRA money, but…who cares? Are the orthopedic surgeons really suffering financially that they can’t afford EHRs? Last I checked, those primary care docs are making a fraction of what the surgeons make and their margin of error – both in terms of available $$ and productivity – are a LOT smaller.
Further, does anyone doubt that it’s in the primary care arena that we stand to gain the most, nationally, from a more efficient system (unless, that is, we start taking the $$ from the specialists…)? How else are we going to deal with the national issues of diabetes, asthma, hypertension, etc.? Socially, we need the primary care docs wired up more than anything.
To Frustrated Farmacist — thank you for a fabulous post. Every hospital building project in the country should go on hold until the planners read what you have written here.
Dumbwaiters always make me think of “Harriet the Spy.” I can see where they’d be quite useful in a hospital, so long as the building is properly designed to accommodate this mode of delivery. However, many care facilities I see in use today would have to seriously reorganize in order to use that system. Interesting that the robot company is out of business: that option looks particularly useful for the sprawling hospitals I’ve been in (plus I can’t help thinking about R2D2 whenever I see one in action).
Evan Steele makes an excellent point: “Without such a system, downtime can become more than an annoyance — it can be a life-threatening event.”
There is need for for data on the adverse events from planned or unplanned downime and the delays that emanate. At present, there is not any data. What are they hiding?