'Samantha Brown points out that, “Healthcare, like every other industry, gets caught up in the idolatry of the ‘innovators.’”' I…
Monday Morning Update 4/12/10
From Thad: “Re: Allscripts. Word is that an inside e-mail leaked out to a wider audience of employees than planned. It mentioned the pending merger of Allscripts with Eclipsys.” Inga tried to chase this rumor down, but of course nobody’s saying anything to confirm or deny. Several people have told us Microsoft will make a move on Eclipsys very soon, but I’m always skeptical about Eclipsys rumors because they come up every year or so. But if you asked me if either event is possible, I’d say yes, even though I don’t see the value in either scenario. ECLP announces results on May 4, which may or may not be relevant.
From J-Hi: “Re: meaningful use. Does anyone know a source that lists the 25 objectives and the comments submitted to CMS for each?”
From Tangelo: “Re: AFCEA military HIT conference. Between the speakers from HHS, VA, and DOD and the large government contractors lining up to suck on the HITECH teats, it’s embarrassing to see how disconnected they all are on the real issues of implementing HIT (meaningful use and HIE) at the community level.”
From PortlyChap: “Re: QuadraMed. Quadramed lost the last of its Affinity clients in Kentucky recently. Pattie A. Clay Regional Medical Center in Richmond recently signed a contract with Meditech. The only other Kentucky Quadramed Affinity client signed a contract with Meditech in December 2009.” Unverified.
Transcription provider Transcend bids $78 million for the bankrupt Spheris, slightly upping the $75 million offer on the table from CBay and Nuance. And in another interesting development, Oracle CEO Larry Ellison is apparently protesting the potential sale of Spheris to that second group because Oracle is a Spheris bankruptcy creditor and he doesn’t want its software transferred to the new owners. The auction for Spheris starts today (Monday).
I’ve almost finished getting the new search engine running. There’s a new “Search This Site” box to your upper right if you want to try it. It indexes all HIStalk-related sites in one search (HIStalk, HIStalk Practice, HIStech Report, and HIStalk Mobile).
I did a survey two years ago in which I asked readers who work for hospitals to tell me their position and where they work, just to give me a feel for who’s out there. I shared the list of hospitals here. It’s time for an update! If you work for a hospital or health system, please complete my survey that asks only three anonymous questions: your job title, your employer’s name, and the city/state it’s in. Thank you.
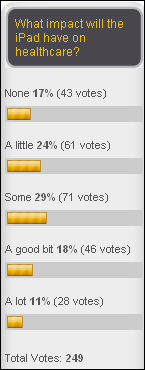
Opinion is mixed on the likely impact of the iPad on healthcare, which is still pretty good considering it’s primarily a consumer device. New poll to your right: which of the big hospital systems vendors is the most innovative?
Clarian Health Partners (IN) chooses MedVentive for its Clarian Quality Partners clinically integrated network, where its product will be used to analyze patient data for quality analysis and care improvement opportunities. Clarian Health Ventures will also invest in MedVentive, jumping into an oversubscribed $10 million Series C funding round that raises the company’s total to $18 million.
Not much has gone right lately at Miami’s Jackson Health System, so maybe this was inevitable. Its Lawson payroll conversion causes most of its employee paychecks to be incorrect, although by minor amounts. Lawson says the problem was in the system it replaced and its amounts are correct; the hospital says the new checks underpaid employees for working overtime.
Some of the rags got irrationally exuberant over the marginal news that McKesson will sell its Asia-Pacific subsidiary to Medibank. The editors should have known better – all that subsidiary does is run healthcare-related telephone hotlines and call centers in Australia and New Zealand. Impact in the US or to McKesson’s bottom line: pretty much zero.
I notice that Cerner shares are on a solid rise lately, including a 2.4% jump Friday. You could have doubled your money if you’d bought in exactly one year ago. Neal’s stake is worth right at a half billion dollars.
Misys turned in pretty good Q3 numbers Thursday, with its Allscripts ownership stake offsetting a soft market for its banking software.
A small but interesting study in Australia finds that informed consent delivered interactively via computer with illustrations and quiz questions improves patient understanding and turns the usual “sign here” paper process into a valuable educational too.
I really enjoyed the discussion about which systems a 200-bed hospital should consider. Here’s the next reader question that would benefit from your feedback: when hospitals are rolling out systems to physician practices, will they offer a menu of a la carte system and implementation options, or will the hospital offer only a standard enterprise model of software and devices? E-mail me your thoughts and I’ll compiled them as a follow-up.
St. Francis Hospital (OH) implements the Priority Consult patient navigation system for its breast care patients. The company, which I hadn’t heard of, has software to support patient-focused nurse navigation models for spine centers and breast care, facilitating intake, triage, and care coordination.
Pardee Hospital (NC) replaces its two forms management solutions with Access Enterprise Forms Management when it finds the original systems couldn’t product a patient wristband barcode small enough for newborns.
Justen Deal follows Canadian HIT more than I do, so he caught this story that I would have missed. Quebec’s opposition party says its EHR project is dead last in all of Canada. The pilot, due to be completed in 2008, “still isn’t working” even though all of Quebec was supposed to be live this year. It appears that 75% of the original $563 million budget has already been spent, critics say it’s going to cost at least $1 billion, and everybody who originally supported it is trying to distance themselves from it. Justen always cites my 2007 Universal Rules for Big EMR Rollouts, saying they should have read them up there, so I’ll repurpose below just in case anyone missed them the first time around.
Speaking of which, I love this Toronto Star article, Malawi’s $1 Million eHealth Miracle. It points out that while Ontario was spending $1 billion on eHealth with “almost zip” results, dirt-poor Malawi has the records of 1.1 million patients accessible in 10 locations throughout the country, thanks to a computer network put together by a non-profit created by a Canadian aid worker and his wife for a total cost of $1 million from their office above a 7/11. He bought obsolete computers from eBay, converted them to touch screens, and developed the patient registration app, which uses “health passports” that cut the hours-long lines. “It’s hot, dusty and hydro is intermittent. Health clinics are in the open air with no doors. We needed a computer system that would work in those conditions and be used by people who don’t have computer skills. The system works on the premise that if you can work a mobile phone, you can use a touch-screen computer.”
A Harvard research team finds that electronic medical records haven’t had much impact in improving care or reducing costs. The authors seem to begrudgingly acknowledge that there’s no turning back now that the government is throwing endless money at EMRs, acknowledging that meaningful use requirements will at least encourage them to be used and not just purchased.
Central Washington Hospital gets a local newspaper writeup for its Cerner go-live. I’ve been there – nice place, lots of apples at the right time of year.
Mr. HIStalk’s Universal Rules for Big EMR Rollouts (From 2007)
1. Your hospital will pledge to make major process changes, vowing to “do it right” unlike all those rube hospitals that preceded you, but the executive-driven urgency to recoup the massive costs means the noble goals will change to just bringing the damn thing up fast, hopefully without killing patients in the process.
2. The project and/or system must be anointed with an incredibly dopey and user-embarrassing name, preferably chosen from user submissions and with the offer of crappy vendor paraphernalia or lame IT junk as a prize, and also preferably made up of a far-fetched phrase whose contrived acronym spells out a medically related word or female name. Instead of inspiring the expected collegial chumminess among users, it will serve as a bitter reminder of the innocent, naive days between RFP and go-live before it got ugly.
3. Doctors won’t use it like you think, if at all, because hospitals are one of few organizations left that doctors can say ‘no’ to.
4. You’ll spend a fortune on mobile devices and carts that will sit parked in a corral due to the short life of their $100 battery and a dysfunctional but not yet fully depreciated wireless network, the keystone arches to the entire project.
5. All the executives who promised undying support to firmly hold the tiller through the inevitable choppy waters and who overrode all the clinician preferences in a frenzy of inflated self esteem will vanish without a trace at the first sign of trouble, like when scarce nurses or pharmacists threaten to leave or when the extent of the vendor’s exaggeration first sees the harsh light of day in some analyst’s cubicle.
6. It will take three times as long and twice the cost of your worst-case estimate.
7. You’ll pay a vendor millions for a software package consisting of standardized business rules, then argue bitterly that all of them need to be rewritten because your hospital is extra-special and has figured out the secrets that have eluded the vendor’s 100 similar customers. The end result, if the vendor capitulates, will be a system that looks exactly like the one you kicked out to buy theirs.
8. You’ll loudly demand that the vendor ship regular software upgrades to fix all the bug issues you submit, but then you’ll refused to apply them because you’re scared of screwing something up with the skeleton maintenance staff you can afford, given that millions were spent on systems with nothing left for additional IT support staff or training.
9. All those metrics you planned to collect to show how quickly the EMR would pay for itself instead show the situation unchanged or getting worse, so factors beyond your control will be blamed (like a ridiculously long implementation time that changed all the assumptions and external conditions) and ROI will not be brought up again in polite company.
10. No matter how unimpressive the final result toward patient care or cost, the EMR will be lauded far and wide as wonderful since the vitality of the HIT industry (vendors, CIOs, consultants, magazines, HIMSS, bloggers) requires an unwavering belief that IT spending alone will directly influence quality, even when nothing else changes.








“Mr. HIStalk’s Universal Rules for Big EMR Rollouts (From 2007)” – absolutely priceless. I love it! Keep up the excellent work.
Central Washington Hospital in Wenatchee, Good luck on the recent Go live and expected outcomes with physician adoption. I hope you can make it work well and at the same time get a bill out the door thats correct without a major manual process. We always seem to forget about that side of healthcare when it comes to Cerner for some reason.
I had lunch with a knowledgeable CIO recently who insisted to me that Cerner’s next big move is to get deep into the hospital management/ownership space. I would normally dismiss something like this but the spiel was just plausible enough to believe. Check it out…
re Wenatchee and COWS—
*She said computers on wheels also allow medical staff to immediately chart critical data “without taking our eyes off our patient. … that is huge.”
/oh the huge manatee…
The name of the Canadian aid worker who built the eHealth infrastructure in Malawi is Gerry Douglas. Not one to toot his own horn, Gerry doesn’t even put his name on the website of the non-profit (Boabob) he founded through which the funding came to get the work done.
Since he won’t do it, I will. Gerry is a true humanitarian, brilliant, affable, and down to earth. Great job, Gerry!
News that you may have missed…
HL7 Pioneer Joachim Dudeck passes
http://ow.ly/1wYd5
Mr. H.,
The truth is finally leaking:
“From Tangelo: “Re: AFCEA military HIT conference. Between the speakers from HHS, VA, and DOD and the large government contractors lining up to suck on the HITECH teats, it’s embarrassing to see how disconnected they all are on the real issues of implementing HIT (meaningful use and HIE) at the community level.”
They too ignore the complaints of the adverse events potentiated by HIT and are a bunch of back slapping good old yes men and women.
Someplace in the world, there is going to be an extensive catastrophe from these ill conceived computerization systems that are being built, deployed, and used in a vacuum of what is safe and accurate for the patients.
EMR Rollouts Rules…Great!
Now I’ll have to expand my Ten Commandments for HIT to 15, but I can’t find stone tablets big enough!
http://histalk2.com/2008/07/27/histalk-guest-writer-frank-l-poggio-and-the-ten-commandments-of-healthcare-information-technology/
In view of the investment, “Clarian Health Ventures will also invest in MedVentive, jumping into an oversubscribed $10 million Series C funding round that raises the company’s total to $18 million. “,
does anyone think that adverse events or glitches will be reported outside of the hospital? Does it have to be another heparin blunder in order to protect patient safety?
Has anyone else noted an increase in how much contractors are charging?
RE: EMR rollout rule #2 (embarrassing names). I worked for a system where the first two letters of the hospital acronym were “F-U”, no kidding. It took all us peons about two seconds to figure this out, but they went ahead and named it anyway. Needless to say, the name has been changed.
RE: HealthcareIdiotSavant: What I’m seeing at my hospital is that if you have a policy in a drawer that conflicts with a policy programmed into a computer, the computer wins. If quality, savings and efficiency are all goals, it’s logical that a big HIT company would want to cut out the middleman and run a hospital itself.
Glad to see your Universal Rules for Big EMR Rollouts™ again. Honestly, if every CEO, CIO, physician, and project manager had to read that before committing to any deployment, we might actually see a few more projects come in at only double their original budget (instead of triple). Imagine the cost savings!
In all seriousness, there are some very invaluable points in there that get lost amongst all the buzzwords and acronyms that drown out most common sense in HIT. I’ve told you this before, but you really could, and should, turn those ten rules into a book.