I want to add the following. I'm an IT professional. In the course of my professional duties, I'm expected to…
Monday Morning Update 4/20/09
From Leonard Smalls: “Re: CIOs. The selection of the HIMSS chair best highlights all that is wrong with healthcare IT. He was an X-ray technician, went to work for a healthcare IT vendor, and then to his hospital, where he is now CIO. He was groomed by vendors and HIMSS with little information technology education and experience other than vendor applications. This is what is wrong with healthcare IT. You can’t be just a good manager and join the right organizations to be an effective CIO. You must have information technology education and real-world experience in the layers below the application layer in order to make effective decisions about systems and how to integrate them. If not, you become a vendor-whore (pardon the language). I see this repeated often in healthcare organizations. Those in the industry need to stand up and shout when the emperor has no clothes. Otherwise, sit down, be quiet, and quit complaining about crappy software in the healthcare IT space.” This is the “CIO as the technician in charge vs. generalist change leader” argument that never seems to end. One camp says hospital CIOs should be doctors and nurses, another says they should be the same kind of person you’d want for COO or even CFO, while the old-schoolers says the CIO should know the bits and bytes. I’ve yet to see a convincing correlation between CIO effectiveness and their background since so much depends on leadership style and the organization they work for. I do believe that hospital CIOs are too cozy with the idea that everything revolves around vendor software, often because that’s all they know. Look at how chummy CIOs are with vendors with HIMSS and CHIME – is that an admirable win-win position or is it an incestuous relationship? Either way, that’s why it’s an uphill battle for open source applications, internal development, or simply optimizing the use of what’s already been bought. Those less-sexy efforts rarely get you on the A-list of advisory boards, speaking engagements, and rah-rah magazines. Plus, lemming hospital executives are swayed by vendorspeak, too (“vision centers” are for non-IT execs looking through a gauzy and deceiving lens, for the most part, not CIOs) and not encouraging their CIOs to blaze any trails.
From Svetlana Stalin: “Re: two million visitors. This very intelligent and sometimes bizarre Web comic strip relates to your recent achievement. Congratulations!” Link.
From Bashkirian: “Re: the data model that nearly killed Joe. Heard the vendor was Epic. Can anyone confirm?” I believe ample clues were provided to draw a conclusion about the vendor, although the conclusions about the magnitude of the problem and who’s to blame for it could certainly vary.
From Speedo: “Re: MED3OOO. Heard Tom Skelton has inked a big deal with Tenet.”
From IT Manager: “Re: Carilion. Carilion Clinic’s EMR implementation is going as smoothly as any I have seen at several other health systems. I think we are rolling out Epic at all of our hospitals and ambulatory sites faster than anywhere else in the US. Carilion’s 140-bed hospital implemented Epic smoothly on all applications just a few months after the 800-bed Carilion Medical Center went live.”

President Obama names 36-year-old Aneesh Chopra as chief technology officer of the United States in his Saturday morning radio address. Chopra is Virginia’s secretary of technology, but more relevant to healthcare, was previously managing director of The Advisory Board Company, the publicly traded healthcare consulting and advisory firm, where he led the CFO group. His LinkedIn profile shows no technology experience or education whatsoever (that should drive Leonard Smalls, whose comment about CIOs is above, crazy), although his Democratic party participation is impeccable. Jeff Bezos, Bill Gates, Eric Schmidt, and other big-name visionaries had been touted for the job, so many are scratching their heads as to why he was chosen and what he brings to the table. HIMSS gave him a state advocacy award in 2007, so I’m sure a fawning press release applauding his selection is imminent. I wouldn’t get too stoked: he’s not a member.
Interesting: Gibson General Hospital finds a Russian hacker’s exploit on its e-mail servers that allowed them to be used to forward spam all over the world. Palisade Systems, whose packet management technology was used to detect and fix the problem, ran the press release. One case study involved using the company’s PacketSure Procotol Management Appliance to limit peer-to-peer traffic for a university.
The latest newsletter (warning: PDF) from Intellect Resources has thoughts on how to tell your kids that you’re out of work (advice you’ll hopefully never need). Check in, too, with Traveling HIT Man (their version of Flat Stanley) to see where he’s been. He may find his way to HIStalk Intergalactic Headquarters someday.
Would you please complete my reader survey? I do it every year to help me keep HIStalk on track. Thanks.
A pharmacy technician whose job was the subject of layoff rumors kills the pharmacy manager, a co-worker, and himself at Long Beach Memorial Medical Center (CA).
Anonymous whistle-blowers claim (and press-obtained documents seem to confirm) that the Australian government is rushing its Cerner systems into production without any medication functions working, presumably to get something live to avoid embarrassment in next year’s elections. The $70 million system was ripped by an unnamed health IT expert, who predicts hospitals won’t use it: “No one likes using it because it’s shit. It’s totally inflexible.”
The folks at Digital Healthcare Conference (May 6-7 in Madison, WI) are offering a special $295 registration rate (use code HISDC) for provider readers of HIStalk. It’s a pretty high-powered speaker list and a nice facility (Fluno Center for Executive Education, above). I’d go if I could get off from work.
Those pink-pantsed boys at Voalte have got their marketing on despite being a start-up. This funny video makes fun of an unnamed competitor that should be obvious to everyone, a la Apple vs. IBM (Voalte isn’t a sponsor or anyone I know, by the way, for those who may think I have a hidden agenda – I just find their product interesting and their approach fresh).
BIDMC CIO John Halamka says sending clinically unreliable administrative data to Google Health for PHR use was a mistake in retrospect, as evidenced by the head-scratching conclusions e-Patient Dave found when he viewed his own records there and found a long list of medical conditions that he mostly didn’t have (but had been tested for). BIDMC is shutting down the ICD9 feed and trying to map their homegrown software’s data to SNOMED-CT instead of sending free text. e-Patient Dave, who is the public face of the problem, is advising Google and BIDMC. Not to minimize his contributions, but couldn’t Google have spent a few of its gazillion dollars to actually talk to one of the many informatics experts in the industry instead of just happily blowing in whatever data BIDMC said it could send and calling it mission accomplished? Honest to God, we’ve got real-life doctors, nurses, informatics PhDs, and nomenclature and taxonomy experts everywhere and nobody ever asks them, instead just sending off a bunch of marketing types and programmers to hack out something that looks cool even if it is somewhere between medically useless and medically wrong. Show of hands: who out there would have told Google that it was a fantastic idea to use claims data as a clinical tool? (like, “The doctor tested you for cancer once, ergo, you must have cancer.”)
If top dogs Google and Harvard’s BIDMC (and Uncle Sam, who’s putting a lot of faith in aggregating data from iffy and undocumented sources) can’t figure out this data quality issue, what does that say about an industry that’s about to spend billions on a national data exchange? Who’s going to validate and correct EMR data that’s being whisked electronically all over the country? (or, more importantly, who will use it knowing its limitations, which is the reason that PHRs are of limited value today?) Here’s what e-Patient Dave wisely said about the fiasco: “I suspect processes for data integrity in healthcare are largely absent, by ordinary business standards. I suspect there are few, if any, processes in place to prevent wrong data from entering the system, or tracking down the cause when things do go awry. And here’s the real kicker: my hospital is one of the more advanced in the US in the use of electronic medical records. So I suspect that most healthcare institutions don’t even know what it means to have processes in place to ensure that data doesn’t get screwed up in the system, or if it does, to trace how it happened.” I was talking to Robert Connely of Medicity (formerly Novo Innovations) and we agreed that interoperability is a piece of cake compared to the next mountain to climb: semantic interoperability (I’m getting this data element from you, but tell me what it really means). Vendors don’t always document that even in their own databases (see the healthcare data model critique that I wrote about earlier).
The Australian Business Journal profiles the resurrection of IBA Health, parent of British software company and NPfIT vendor iSoft. Some fun talk from IBA’s chairman about that iSoft acquisition, which initially was going the other way as the much larger iSoft was to acquire IBA, but then iSoft’s market cap dropped from $3 billion to $300 million. “It had lost 90 per cent of shareholder value and its management team and we ended up as the underdog bidder — the pissy little Australian company — wanting to take over a British institution. They did not treat us seriously. I guess there was a bit of colonialism involved. They had hoped an American company would take them over. Instead, I came back with a slingshot and we took it over.”
Speaking of IBA, it acquires Hatrix, an Australian vendor of eMAR systems.
Alaska, already the most pork-heavy state, zips through a bill pushing electronic medical records, hoping to grab some stimulus money.
A Huffington Post article by Deane Waldman (a doctor) decries poor usability in clinical systems. “I can access my Excel spreadsheets on either MAC or PC but I cannot see a chest X-ray and lab results using the same program. Inpatient files are coded (and secured) separately from outpatient records making it impossible easily to compare them … The Obama administration is encouraging the development of EMR and that is wonderful. The scary part is that I know they will do it wrong. They will do ‘business as usual’ … As a colleague on Twitter wrote recently, ‘IT tends to focus on back-end programming and loses sight of the front-end [the users]. Without usability, software is [and EMR will be] useless’ … the screen in the hospital on which I am supposed to electronically sign my letters: it has 74 icons! Talk about incomprehensible. The needs of the end-users must drive the design.”
CCHIT takes the first step toward its expansion to certify long term care systems, putting together a LTCS Advisory Task Force. The CCHIT apple didn’t fall far from the HIMSS tree: keep the paid headcount down, use volunteers to do all the real work, keep expanding, and figure out multiple revenue streams. None of that is bad, necessarily.
GE’s Q1 earnings sucked less than expected: EPS $0.26 vs. $0.43, but the GE Capital news just keeps getting worse: its earnings dropped 58% to $1.12 billion, but without a favorable, one-time tax treatment, it would have lost $153 million. GE Healthcare wasn’t exactly a bright spot, with revenue down 9% and profits off 22%.
Reading Hospital (PA) will lay off 250 employees.
Turns out the cure for the nursing shortage was a recession. The RN position vacancy rate in Massachusetts is only 4%, with new grads scrambling to try to find jobs. Mass General has a 2% vacancy rate, BIDMC is laying off some nurses, and Children’s has nothing for new grads.
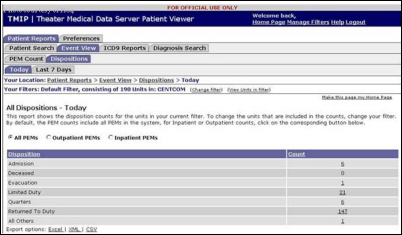
Top military doctors in Iraq aren’t happy with its new tracking system for wounded soldiers. The new system, Theater Medical Data Store (TMDS) replaced Joint Patient Tracking Application (JPAT). I wrote about JPAT awhile back, citing this article and others. Lt. Col. Mike Fravell was a Landstuhl Regional Army Medical Center CIO and VA fellow who built JPAT himself, where it found a wide and appreciative user audience, but his initiative annoyed top brass determined to spend big money on the TMDS replacement system. He was transferred out to his own Siberia. The main complaints about TMDS involve data loading time (it’s run from servers in Virginia) and multiple information links for each patient, making easy interpretation difficult. An army vascular surgeon sounds like his civilian counterparts: “I know JPTA is dead, but our current system is not functional. As we do more with less putting the administrative burdens on the doctors is ludicrous.”
Odd lawsuit: a woman is suing Boulder Community Hospital (CO) and nearly a dozen doctors, claiming that the hot water bottle placed underneath her while she was in labor exactly two years ago left third-degree burns on her buttocks.






Re: debate on CIOs; as a professional who has made a 2+ decade career as a “rent-a-CIO” – I have found that the skill mix required is intimately tied to the culture of the Organization and the engagement of the Board.
However, one trend I suspect is coming quickly and which the last time this trend became reality, HCIT slipped from ~4% of OPEX to >2% – and that is, in times of financial stress (like now) Health Systems seem to tilt towards promoting into the CIO slot from within; afterall this avoids a possible extended time w/o and avoids recruiting fess.
Given this behavior it would seem that 2 possible trails: (1) – many CIOs do a terrible job of succession planning; (2) – those holding the financial strings do not value the CIO to the extent we would all wish for.
Re: Why not talk with Medical Informatics Vocabulary Experts? I believe it is because the builders of the systems and their clients don’t want to hear the answer and do the work. There are billions of records that would have to be cleaned and work-arounds and walls to isolate potentially “unclean” data. There is also a tremendous amount of retraining to do. All the clinicians who were trained to document one way, with one set of vocabularies (or lack thereof) will need to learn a new set of vocabularies. These are sometimes very poorly implemented (a la “The Data Model That Nearly Killed Joe”).
By the way, the is alive and doing well. Have an unconfirmed and unsupportable report that a new EMR is entering the market; ShamWow ERM. You following me IT guy?
Understand that predictive analytics data modeling is the premise for this novel approach to structure semantic patient data; don’t be confused by any other ShamWow EMR look- alike!
Thought that I was being censored! The Bugajski Phenomenon is alive and doing well. Talk about beating a dead horse.
Since CIO stands for – Carreer Is Over…what does it really matter? You don’t like the one that’s there now? Well hold your breath, it shiouldn’t take long.
My daughter is in a BSN program in Boston and has already been told to think away from Boston after graduation. Good news is we dont come from the Eastern Mass area and she has no strong desire to practice there after graduation.
I think there is a micro climate in the Boston Area that does not reflect the national picture. There are still plenty of prime RN/BSN acute hospital positions across the country remaining unfilled. There has been a contraction for sure due to the economy that has dried up a proportion of open FTE’s but the overall demographic trends still dont give cause to have reduced overall concern about the lack of nursing talent in the coming years.
Aging oomer population growing, nursing faculty retiring en mass, average age of RN’s in the mid to high 40’s…you do the math!
“I’ve yet to see a convincing correlation between CIO effectiveness and their background since so much depends on leadership style and the organization they work for.”
I respect your opinion and usually agree with your comments. But not this one.
Would you hire a general contractor to construct a building who is a generalist change leader with experience in a related field but none in the “bits and bytes” of constructing a building? Or one that has spent years constructing buildings, working their way up the organization, gaining experience managing other contractors?
You need a leader with a technical background. Is that too much to ask for?
[From Mr. HIStalk] The worst CIOs I’ve seen had a strong technical background. It’s great if it’s a five-person IT shop and they’re just a glorified programmer or network engineer. The bigger the IT organization, the less that matters. In a 200-person IT shop, the worst way to spend $200K or more on a CIO is to expect them to work alongside $60K programmers. That’s what supervisors or managers are for, which are usually at least 1-2 levels below CIO.
“In a 200-person IT shop, the worst way to spend $200K or more on a CIO is to expect them to work alongside $60K programmers.”
I agree. That’s why you need a “Leader” WITH “bits/bytes” skills. Not just one or the other. Thats the point.
Question: If Aneesh Chopra is the CTO, then why have a CIO (Vivek Kundra)? Is there anything different between these 2 jobs, or are they political paybacks?
BTW, big gossip that you may have missed (I didn’t think that possible)! In case you didn’t know, last month Mr. Kundra, shortly after being appointed as CIO, he had to step down because the office where he came from got raided by the FBI with 2 of his former associates charged with “bribery of a public official, money laundering, wire fraud and conflict of interest”. URL: http://www.huffingtonpost.com/2009/03/12/fbi-raids-obama-technolog_n_174265.html He has since been reinstated.
Superb perspective on the data transfer / data models issue. Possibly the best concise-but-comprehensive recap of the facts & implications I’ve seen.
I’m so happy to see data professionals getting involved in this. I particularly recommend last Wednesday’s post on IQTrainwrecks.com.
Last week in preparation for our call with Google Health and my hospital, my primary doc spent hours digging through all my records, cross-referencing who did what when, as best he could determine, and double-checking whether there was any shred of evidence for various odd billing codes. Last night I posted the outcome. Not only are there things that look like sloppy miscodings, there were some things that bear no relation to reality: 733.90 Bone & Cartilage Disease during a visit for a lump growing out of my tongue, 733.13 Pathological Fracture of Vertebrae (no such diagnosis ever made), armpit cysts diagnosed during an abdominal ultrasound, etc.
My post detailing those items is here. Aside from the need to get real about data quality, my message to patients (including you!) is that we better get moving on clean-up: in some cases these errors could give seriously wrong info to a doc who picks you up in an emergency.
TPD is truly amazed at the types of mistakes in e-Patient Dave’s EMR and can see how creating a PHR with bad data could be the worst thing for a patient’s next present. One method of preventing bad billing codes from being entered into a PHR is to be selective with your data mining efforts so billing info is segregated from true treatment experiences and then matched with what actually happened with the patient conditions and treatment.
This whole debate on whether a tech background vs. a medical background make a good CIO misses the point. To be a good CFO, you need a balance between business leadership, accounting/finance principals, industry experience and vision. To be a good CIO, you need a balance between business leadership, technology experience, industry experience and vision. Candidates come to the table with different strength areas (no one is fully developed in one area), which is why some CIOs with no tech background are incredibly effective and why some with no healthcare background are also incredibly effective. The key is to be balanced, to have people on the team who fill in weak spots, and use those people.
John O.
John Overbaugh Says:
“To be a good CFO, you need a balance between business leadership, accounting/finance principals, industry experience and vision.”
I agree with your statement about balance. But would you consider hiring a CFO without an Accounting undergrad? Unlikely. So why not have a similar requirement of a CIO, an undergrad in computer engineering or computer science. And to support what you said, other factors like leadership, industry experience, vision.
A CIO with no tech background is the same as a CFO with no accounting background. Or it should be the same.
I doubt that healthcare organizations would hire a CFO or CNO without the appropriate education and experience backgrounds, which I believe extends to the CIO position. Without this background, CIO are dependent on subordinates, vendors, consultants or others for knowledge and understanding of technical issues and are not able to bring their own knowledge to these issues. As with nurses, accountants and workers in general, IT personel expect their leadership to have an understanding of their work and will test leaders to determine thier knowledge and understanding of IT. But, this knowledge and experience is only one aspect of a good CIO. In addition, a good CIO must have good leadership skills, which are not easily defined or acquired. I would think that effective CIO’s don’t need a balance between technical knowledge and leadership skills, since they aren’t mutually exclusive, but a deep understanding of both aspcts and the ability and desire to apply both aspects effectively.
Well said, Bilbo.
Well said, Bilbo.